Why is my tongue white? If you have ever looked in the mirror and noticed a white coating or patchy white spots on your tongue, you are not alone — it is one of the most searched oral health questions online. In most cases a white tongue is harmless and clears up on its own with simple oral hygiene changes.
But in some situations it is your body’s way of signaling something that needs medical attention.
Why Is My Tongue White? The Simple Biology First
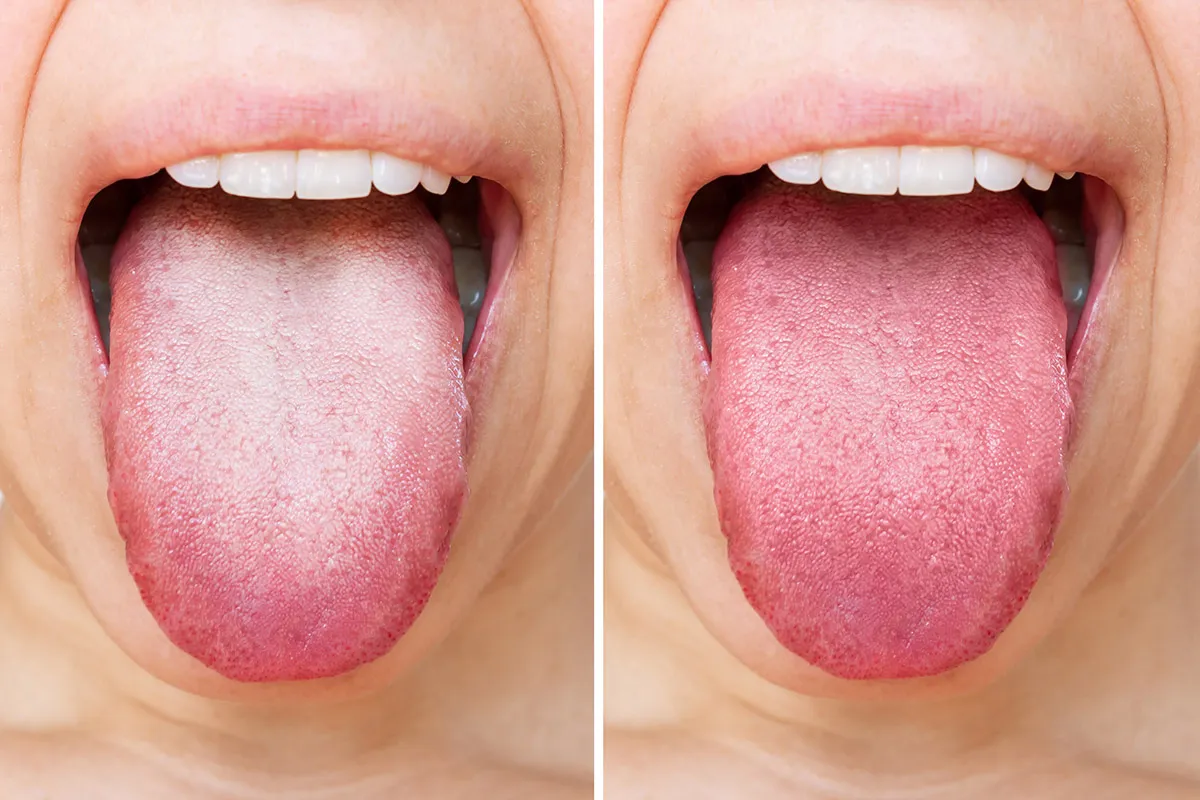
Your tongue is covered with tiny finger-like projections called papillae. These papillae are responsible for your sense of taste and texture.
When the papillae become inflamed, swollen, or enlarged, they create microscopic pockets where bacteria, dead cells, and food debris get trapped. That trapped material is what creates the white or off-white coating you see.
In most cases the buildup is superficial and clears easily. In other cases the white appearance comes from a specific condition — and knowing the difference matters.
The 9 Main Reasons Your Tongue Looks White
Poor Oral Hygiene and Tongue Buildup
This is the single most common reason for a white tongue in otherwise healthy adults.
When you skip brushing your tongue or never use a tongue scraper, bacteria and food particles accumulate on the papillae rapidly. The coating can appear thick, yellowish-white, and may come with bad breath.
The fix is straightforward: brush your tongue from back to front after every brushing session, or use a dedicated tongue scraper daily. Most people see visible improvement within 24 to 48 hours.
Dehydration and Dry Mouth
Saliva is your mouth’s natural cleaning system. It constantly washes away bacteria, dead cells, and debris from the tongue surface.
When saliva production drops — due to dehydration, certain medications, or a medical condition called xerostomia — bacteria multiply unchecked on the tongue. The result is a dry, white-coated tongue that may also feel sticky or rough.
Drinking at least six to eight glasses of water daily supports healthy saliva flow. Chewing sugar-free gum between meals also stimulates saliva production.
Mouth Breathing
People who breathe predominantly through their mouth — especially during sleep — experience accelerated drying of the tongue and oral tissues.
Overnight mouth breathing allows moisture to evaporate from the tongue surface, leaving a white or patchy coating by morning. This is one of the most common explanations for waking up with a white tongue every day.
Using a humidifier in the bedroom, treating nasal congestion, or addressing underlying sleep apnea can significantly reduce this effect.
Oral Thrush (Candida Infection)
Oral thrush is a fungal infection caused by an overgrowth of Candida albicans — a yeast that normally lives in the mouth in small amounts.
When the balance is disrupted, Candida multiplies and forms creamy white or yellowish patches on the tongue, inner cheeks, and roof of the mouth. The patches may look like cottage cheese and, importantly, they can be wiped off — but the tissue underneath is red and sore.
People most at risk include those using broad-spectrum antibiotics, inhaled corticosteroids for asthma, oral steroids like prednisone, or anyone with a weakened immune system, diabetes, or dentures.
Treatment involves antifungal medications — either a liquid you swish around the mouth (nystatin) or an oral tablet (fluconazole). Completing the full course of treatment is essential even after symptoms improve.
Leukoplakia
Leukoplakia produces thick, firm white patches on the tongue, gums, or inside of the cheeks that cannot be wiped or scraped off. This is a key diagnostic difference from oral thrush.
The exact cause is not fully understood, but long-term tobacco use — both smoked and smokeless — is strongly linked to the majority of cases. Heavy alcohol consumption and chronic irritation from broken teeth or poorly fitting dentures are also contributing factors.
Most leukoplakia patches are benign, but a small percentage can become precancerous over time. For this reason, any persistent white patch that cannot be removed should be evaluated by a dentist, who may recommend monitoring or a tissue biopsy.
Oral Lichen Planus

Oral lichen planus is a chronic inflammatory condition that causes distinctive lacy, web-like white lines or patches inside the mouth, including on the tongue.
It is believed to be related to immune system dysfunction, where the immune system mistakenly attacks the cells of the oral mucosa. The most common form — reticular lichen planus — often causes no pain and many people do not even know they have it until a dentist spots it during a routine exam.
A more severe erosive form can cause red, swollen, painful tissue and open sores. Treatment includes topical corticosteroids, steroidal mouthwashes, and antihistamines to manage symptoms. There is no permanent cure, but the condition can be managed effectively.
Geographic Tongue
Geographic tongue is a harmless, benign condition where smooth red patches appear on the tongue surrounded by white or light-colored borders, creating a map-like appearance that changes location over time.
The patches form when small areas of the tongue lose their papillae temporarily. The cause is not fully understood, but hormonal changes, stress, and certain nutritional deficiencies may play a role.
Geographic tongue does not cause long-term damage and does not become cancerous. However, it can cause sensitivity or mild discomfort when eating acidic, spicy, or salty foods. No treatment is typically needed unless symptoms are bothersome.
Hairy Tongue
Hairy tongue sounds alarming but is almost always harmless. It occurs when the filiform papillae on the tongue grow unusually long — up to 18 mm in some cases — and trap dead cells, bacteria, food, and sometimes pigment from coffee, tea, or tobacco.
The tongue can appear white, brown, or even black depending on what is trapped in the elongated papillae. It looks like the tongue has grown a fuzzy coating or short hairs.
Risk factors include heavy smoking, poor oral hygiene, excessive coffee or tea consumption, dry mouth, and the use of certain antibiotics or antacids. The condition typically resolves with improved oral hygiene, increased water intake, and quitting smoking.
Syphilis and Other Infections
In rare cases, a white tongue is linked to a systemic infection. Syphilis, a sexually transmitted infection caused by bacteria, can produce white patches in the mouth during its secondary stage.
Scarlet fever, a bacterial infection, causes a distinctive condition called strawberry tongue — where the tongue appears coated in white with red bumps poking through, then peels to leave a bright red surface.
If you have a white tongue alongside other symptoms like fever, rash, sore throat, or swollen lymph nodes, a doctor should evaluate you promptly for systemic infection.
What Your White Tongue Is Telling You: A Visual Guide
The appearance and location of the white coating or patches gives important clues about the underlying cause.
| Appearance | Location | Most Likely Cause |
|---|---|---|
| Thick white coating, wipes off easily | All over tongue | Poor hygiene or dehydration |
| Creamy white patches, wipe off leaving red sore tissue | Tongue, cheeks, palate | Oral thrush (Candida) |
| Thick white patches, cannot be wiped off | Tongue, cheek lining | Leukoplakia |
| White lacy lines or web-like pattern | Tongue and inner cheeks | Oral lichen planus |
| Red patches with white borders, map-like | Tongue surface | Geographic tongue |
| Fuzzy or hair-like white coating | Top of tongue | Hairy tongue |
| White coating with red bumps | Entire tongue | Scarlet fever (strawberry tongue) |
| White patches with ulcers and rash | Tongue and cheeks | Syphilis (secondary stage) |
Is Your White Tongue Harmless or Serious? How to Tell
Most white tongue cases are benign. But specific warning signs indicate a need for professional evaluation.
Signs It Is Probably Harmless
The white coating wipes off easily with a cloth or tongue scraper. It is not painful and does not cause difficulty swallowing. It appeared after a night of mouth breathing or a day of poor hydration. It is not spreading or getting thicker. It clears within a few days of improved oral hygiene and hydration.
Signs You Should See a Doctor or Dentist
These specific symptoms require professional evaluation without delay.
| Warning Sign | Why It Matters |
|---|---|
| White patches that cannot be scraped off | Could indicate leukoplakia or serious infection |
| White coating lasting longer than 2 weeks | Rules out benign causes, needs diagnosis |
| Pain, burning, or soreness under the white patches | Possible oral thrush or erosive lichen planus |
| Difficulty swallowing or moving the tongue | Could indicate spreading infection or abscess |
| Unexplained weight loss alongside white tongue | Requires full medical workup |
| Bleeding underneath or around the patches | May indicate malignancy |
| White tongue with fever, rash, or swollen nodes | Possible systemic infection like syphilis |
| White patch in a person who smokes heavily | Leukoplakia must be ruled out |
Why Is My Tongue White in the Morning?
Waking up with a white tongue every morning is one of the most common complaints — and it is almost always explained by two straightforward factors.
First, saliva production naturally drops during sleep. Less saliva means less natural cleansing of the tongue surface. Bacteria multiply overnight unchecked.
Second, many people breathe through their mouths during sleep — especially when congested — which dries out the tongue surface even further. The combination creates the ideal environment for that white morning coating.
Brushing your tongue immediately after waking up typically removes it within seconds. If it does not budge, does not improve over several days, or feels painful, it warrants a closer look.
White Tongue in Babies and Young Children
In infants under 6 months, a white tongue after feeding is usually just milk residue — completely harmless and not a cause for concern.
However, if the white coating is thick, creamy, and appears on the cheeks or palate, it may be oral thrush. Oral thrush is common in newborns and infants because their immune systems are still developing. A pediatrician can confirm the diagnosis and prescribe a gentle antifungal liquid.
In older children, white tongue causes are similar to adults: poor oral hygiene, dehydration, or mouth breathing during sleep.
White Tongue and Bad Breath: The Connection
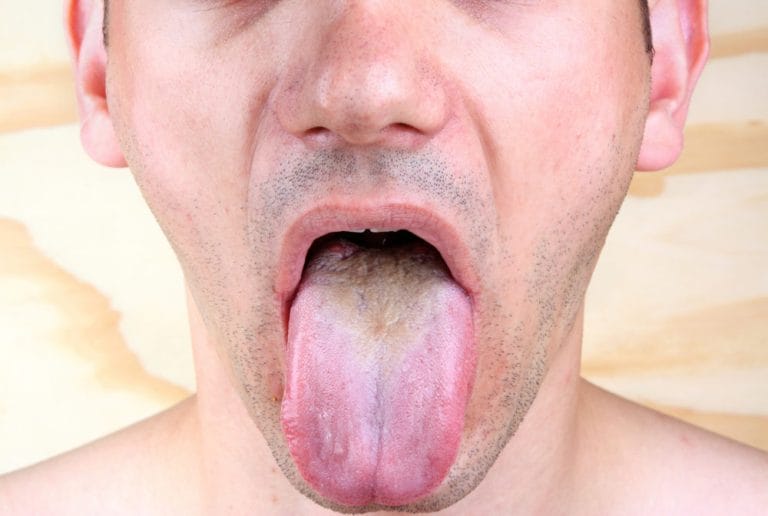
White tongue and bad breath are almost always connected. The bacteria and dead cells trapped between swollen papillae produce volatile sulfur compounds — the primary chemical cause of bad breath.
This is why targeting the tongue directly is one of the most effective strategies for improving breath. Brushing the teeth alone leaves the vast majority of the tongue’s bacterial load untouched.
A tongue scraper removes significantly more bacteria and debris than a toothbrush alone. Studies have shown that regular tongue scraping can reduce bad breath markers by up to 75%.
Conditions That Increase Your Risk of White Tongue
Certain underlying health conditions and lifestyle factors make white tongue significantly more likely.
| Risk Factor | How It Contributes |
|---|---|
| Antibiotic use | Kills good bacteria, allows Candida to overgrow |
| Diabetes | Elevated blood sugar promotes fungal growth |
| HIV/AIDS or cancer treatment | Weakened immunity increases thrush risk |
| Denture use | Yeast hides in denture material if not cleaned |
| Heavy tobacco use | Irritates tissue, promotes leukoplakia |
| Heavy alcohol use | Dehydrates tissues, disrupts oral flora |
| Asthma inhalers (corticosteroids) | Deposits residue that promotes Candida growth |
| Dry mouth medications | Antihistamines, antidepressants, diuretics all reduce saliva |
| Stress | Weakens immune response, disrupts oral bacteria balance |
| Nutritional deficiencies | Low iron, B vitamins weaken mucosal tissue |
Home Remedies That Actually Work for White Tongue
For most cases of white tongue caused by lifestyle factors, these evidence-based home strategies produce quick, visible results.
Tongue Scraping
Use a dedicated tongue scraper every morning before eating or drinking. Gently drag it from the back of the tongue to the front, rinsing between each pass. This removes significantly more debris than a toothbrush and is considered the gold standard for tongue hygiene.
Tongue Brushing
If you do not have a tongue scraper, brush your tongue gently with a soft-bristle toothbrush after brushing your teeth. Use light pressure and work from back to front. This alone can dramatically reduce the white coating within 48 hours.
Salt Water Rinse
Mix half a teaspoon of salt into a glass of warm water and swish for 30 seconds before spitting. Salt reduces bacterial load, draws fluid away from swollen tissue, and creates an inhospitable environment for yeast. Repeat twice daily for best results.
Stay Fully Hydrated
Drink at least 6 to 8 glasses of water per day. Proper hydration supports saliva production, which naturally cleanses the tongue throughout the day. Avoid relying on coffee, tea, or alcohol — all three dehydrate oral tissues.
Probiotics
Consuming probiotic-rich foods like yogurt with live cultures, kefir, or taking a daily probiotic supplement can help rebalance the oral microbiome. This is particularly effective after antibiotic use, when the natural bacterial balance is disrupted and yeast can overgrow.
Reduce Tobacco and Alcohol
Both tobacco and alcohol are primary triggers for tongue discoloration, dehydration, and long-term tissue damage. Reducing or eliminating these significantly lowers the risk of white coating, leukoplakia, and oral infections.
Oil Pulling
Oil pulling — swishing a tablespoon of coconut oil in the mouth for 10 to 15 minutes — has some evidence supporting its antibacterial properties. Coconut oil contains lauric acid, which disrupts the cell membranes of bacteria and Candida. It is not a replacement for brushing but can be a supportive addition.
What to Avoid When You Have a White Tongue
These common mistakes can delay healing or worsen the underlying condition.
Avoid scraping too aggressively — excessive pressure damages the papillae and the mucosal surface. Avoid alcohol-based mouthwashes, which dry out the tongue and worsen the buildup. Do not ignore a white patch that cannot be removed — this always warrants professional evaluation. Do not assume oral thrush will resolve without treatment — it requires antifungal medication. Avoid spicy and acidic foods if your tongue is already sore, as they irritate inflamed tissue further.
Professional Treatments for White Tongue

When home care is not enough, dentists and doctors have effective treatment options depending on the cause.
Antifungal Medications for Oral Thrush
The standard treatment is nystatin suspension — a liquid swished around the mouth four times a day. For more severe or systemic cases, fluconazole tablets are prescribed. Denture wearers should soak dentures overnight in antifungal solution to eliminate yeast hiding in the material.
Corticosteroids for Oral Lichen Planus
Topical corticosteroid gels or steroidal mouthwashes reduce inflammation and manage the burning symptoms of erosive lichen planus. Steroid sprays are an alternative for patients who find mouthwashes uncomfortable.
Monitoring and Biopsy for Leukoplakia
A dentist will typically photograph and monitor leukoplakia patches at regular intervals. If a patch changes in appearance, grows, or shows suspicious features, a tissue biopsy is performed to rule out precancerous or cancerous changes. Quitting tobacco is the single most important step in managing leukoplakia.
Antibiotics for Syphilis
If syphilis is causing white patches, penicillin remains the standard and highly effective antibiotic treatment. All sexual partners should also be evaluated and treated.
Long-Term Prevention of White Tongue
Keeping your tongue consistently healthy comes down to a few sustainable daily habits.
Brush your tongue every single day — morning and night. Use a tongue scraper at least once daily for deeper cleaning. Drink water consistently throughout the day rather than in large amounts at once. Limit tobacco and alcohol to reduce chronic irritation and drying. Schedule dental cleanings every six months so early changes are spotted before they develop. If you use an inhaled corticosteroid, rinse your mouth with water immediately after each use to prevent Candida buildup. Eat a balanced diet with adequate iron, B vitamins, and vitamin C to keep mucosal tissue strong and resilient.
Frequently Asked Questions
Why is my tongue white every morning when I wake up?
Saliva production drops during sleep, allowing bacteria to multiply on the tongue surface. Mouth breathing overnight further dries out the tissue. Brushing your tongue in the morning removes the coating instantly in most cases.
Can a white tongue be a sign of something serious?
Usually no — most white tongues are caused by poor hygiene or dehydration. However, white patches that cannot be scraped off, persist beyond two weeks, or come with pain and difficulty swallowing do require professional evaluation to rule out leukoplakia, thrush, or rarely, oral cancer.
Is oral thrush contagious?
Oral thrush itself is not easily spread between healthy adults, but the Candida fungus can be transmitted through saliva. Avoid sharing cups, utensils, or kissing when active thrush is present, particularly around infants or people with weakened immune systems.
How do I know if my white tongue is thrush or just coating?
Oral thrush patches can be wiped off with a cloth, leaving behind red or sore tissue underneath. A general white coating from poor hygiene or dehydration wipes off evenly without leaving inflamed tissue. If wiping reveals raw, red spots — see a dentist or doctor.
Why does my tongue stay white even after brushing?
If brushing teeth alone does not help, you likely need to brush or scrape the tongue directly. If the white coating still does not improve after consistent tongue cleaning and good hydration for one to two weeks, it may be a condition like leukoplakia or lichen planus that requires professional diagnosis.
Can dehydration alone cause a white tongue?
Yes. Low fluid intake reduces saliva production, allowing bacteria, dead cells, and food debris to accumulate on the tongue surface. Simply increasing water intake and adding tongue cleaning can resolve dehydration-related white tongue within a day or two.
Is a white tongue linked to gut health?
There is a growing body of evidence suggesting that imbalances in the gut microbiome can influence oral health, including tongue coating. An unhealthy gut may promote Candida overgrowth systemically. Adding probiotic foods or supplements can improve both gut and oral bacterial balance.
Should I be worried about white tongue if I smoke?
Yes — smokers should take white tongue seriously and have any persistent white patches evaluated by a dentist. Smoking is the primary risk factor for leukoplakia, a condition where white patches can occasionally become precancerous. Early detection makes a significant difference in outcomes.
What vitamins are linked to white tongue?
Deficiencies in iron, vitamin B12, and folate are associated with tongue changes including white coating, smooth patches, and soreness. These nutrients are essential for maintaining the integrity of the mucosal tissue that lines the tongue.
How long does it take for white tongue to go away?
A white tongue caused by poor hygiene or dehydration typically improves within 1 to 3 days of consistent tongue cleaning and proper hydration. Oral thrush usually resolves within 7 to 14 days of antifungal treatment. Conditions like leukoplakia or lichen planus require ongoing management rather than a fixed resolution timeline.
Conclusion
Why is my tongue white? In the vast majority of cases the answer is simple — bacteria, dead cells, and food debris are building up between inflamed papillae due to inadequate tongue cleaning, insufficient hydration, or mouth breathing.
These causes are easy to fix and respond quickly to basic oral hygiene improvements. But some white tongue presentations are signals your body is sending about something deeper: a fungal infection that needs antifungal medication, a precancerous patch that needs monitoring, an inflammatory condition that needs immune management, or a systemic infection that needs treatment.
The rule of thumb is straightforward — if your white tongue clears within a few days of improved hygiene and hydration, it was almost certainly benign.
If it persists beyond two weeks, cannot be scraped off, causes pain or difficulty swallowing, or is accompanied by other symptoms, see a dentist or doctor promptly.
Early evaluation is always faster, simpler, and far less costly than waiting for a condition to progress. Your tongue is one of the most informative windows into your overall health — pay attention to what it is telling you.
