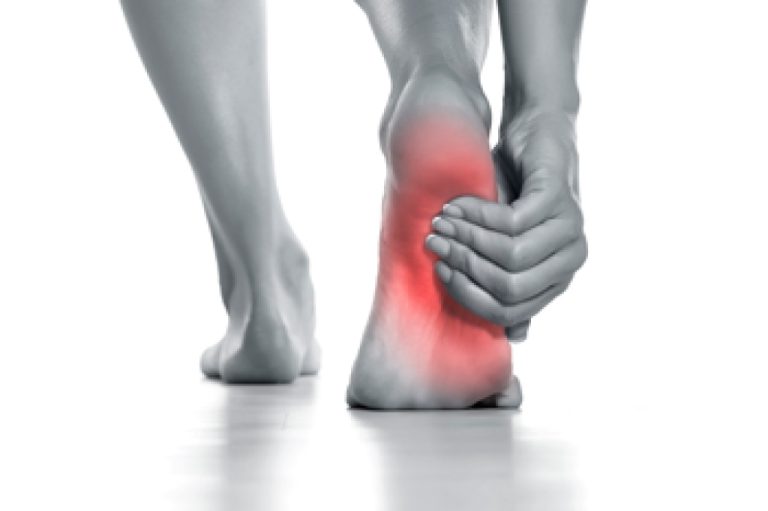
Why does the bottom of my foot hurt is one of the most searched health questions — and for good reason. Foot pain affects millions of people every year, making even simple activities like walking or standing feel unbearable.
The bottom of the foot is a complex structure of bones, tendons, ligaments, and nerves, and pain here can come from a wide range of causes.
Understanding the Bottom of the Foot
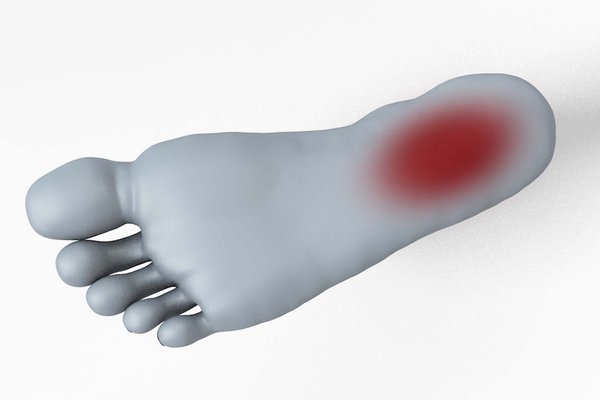
The bottom of your foot — called the plantar surface — runs from your heel to the ball of your foot and toes. It contains the arch, the plantar fascia, metatarsal bones, fatty heel pad, and multiple nerve pathways.
Every step you take puts pressure on this area. The average person takes between 6,000 and 8,000 steps per day, which means your feet absorb enormous amounts of force daily.
When any structure in this area is damaged, inflamed, or under too much stress, pain in the bottom of the foot is the result.
Why Does the Bottom of My Foot Hurt? Most Common Causes
Pain in the bottom of the foot can originate from several different locations — the heel, arch, or ball of the foot. The location of your pain is often the clearest clue to what is causing it.
| Location of Pain | Most Likely Cause |
|---|---|
| Heel (bottom, front edge) | Plantar fasciitis |
| Heel (center or back) | Heel spur, stone bruise |
| Arch (middle of foot) | Flat feet, plantar fasciitis, tarsal tunnel |
| Ball of foot (behind toes) | Metatarsalgia, Morton’s neuroma |
| Entire bottom | Peripheral neuropathy, diabetes-related nerve damage |
| Big toe joint area | Sesamoiditis, gout |
Understanding where exactly the bottom of your foot hurts helps narrow down the cause significantly before seeing a doctor.
Plantar Fasciitis: The Leading Cause
Plantar fasciitis is the number one cause of pain in the bottom of the foot. It affects more than 2 million people in the United States every year, and roughly 1 in 10 people will develop it at some point in their life.
The plantar fascia is a thick band of tissue that runs along the bottom of your foot, connecting the heel bone to the toes. It supports the arch and absorbs shock with every step.
When this tissue becomes overstretched or overused, it gets inflamed and causes stabbing pain — especially near the heel.
Symptoms of Plantar Fasciitis
The hallmark sign is sharp heel pain first thing in the morning when you take your first steps out of bed. The pain often improves after a few minutes of walking, then may return after prolonged standing or activity.
Other symptoms include a burning or aching sensation along the arch of the foot, stiffness around the heel, and pain that gets worse after — not during — exercise.
Who Gets Plantar Fasciitis?
| Risk Factor | Why It Increases Risk |
|---|---|
| Flat feet or high arches | Abnormal foot mechanics strain the fascia |
| Obesity or weight gain | Extra load on the plantar tissue |
| Running or jumping sports | High-impact repetitive stress |
| Standing jobs (nurses, teachers) | Prolonged pressure on the heel |
| Age 40–60 | Fascia loses elasticity over time |
| Tight calf muscles | Pulls excessively on the heel cord |
| Worn-out or flat footwear | Lack of arch support and cushioning |
Women are slightly more likely than men to develop plantar fasciitis. The condition is also more common in people who suddenly increase their physical activity level.
Heel Spurs
A heel spur is a bony growth that develops on the underside of the heel bone. It forms over time as a reaction to stress and inflammation — often as a result of plantar fasciitis pulling repeatedly on the heel.
Most people with heel spurs have no pain from the spur itself. Pain is usually caused by the surrounding inflammation rather than the bone growth.
Heel spurs can be seen on X-rays and are found in people both with and without plantar fasciitis. Do not assume a heel spur is causing your pain just because it shows up on imaging.
Treatment for heel spurs is the same as for plantar fasciitis — rest, orthotics, stretching, and anti-inflammatory medication.
Metatarsalgia: Ball of Foot Pain
Metatarsalgia is the medical term for pain and inflammation in the ball of the foot — the padded area just behind the toes. It is especially common in runners, jumpers, and people who wear high heels or tight shoes.
The pain is typically described as a sharp, aching, or burning sensation. Many people say it feels like walking on a small pebble or stone that is constantly pressing upward.
Common Causes of Metatarsalgia
High-impact sports are a leading trigger. Distance runners place heavy and repeated force on the forefoot with every stride, making them particularly vulnerable.
Foot shape also plays a role. A high arch shifts more pressure onto the metatarsal heads. A second toe that is longer than the big toe causes an uneven weight distribution that stresses the second metatarsal bone.
Excess body weight, hammertoes, and bunions all increase the risk of developing metatarsalgia over time.
Treatment for Metatarsalgia
Rest and reduced activity are the first steps. Switching to supportive, well-cushioned footwear with a wider toe box relieves pressure on the ball of the foot.
Metatarsal pads or cushioned insoles placed inside the shoe can redistribute pressure away from the painful area. Over-the-counter anti-inflammatory medications like ibuprofen help reduce swelling.
In persistent cases, a podiatrist may recommend custom orthotics or corticosteroid injections. Surgery is rarely needed but is an option for severe deformity-related metatarsalgia.
Morton’s Neuroma
Morton’s neuroma is a thickening of the nerve tissue between the third and fourth toes. It causes sharp, burning pain in the ball of the foot and can produce a sensation of numbness or tingling in the toes.
Some people describe it as feeling like a lump or a rolled-up sock inside the shoe. The pain typically worsens with tight footwear and improves when shoes are removed.
It develops when two bones repeatedly rub together and compress the nerve between them. Women who wear narrow, pointed, or high-heeled shoes are at higher risk.
Treatment includes wider shoes, metatarsal pads, corticosteroid injections, and in some cases a small surgical procedure to remove the thickened nerve tissue.
Flat Feet (Fallen Arches)
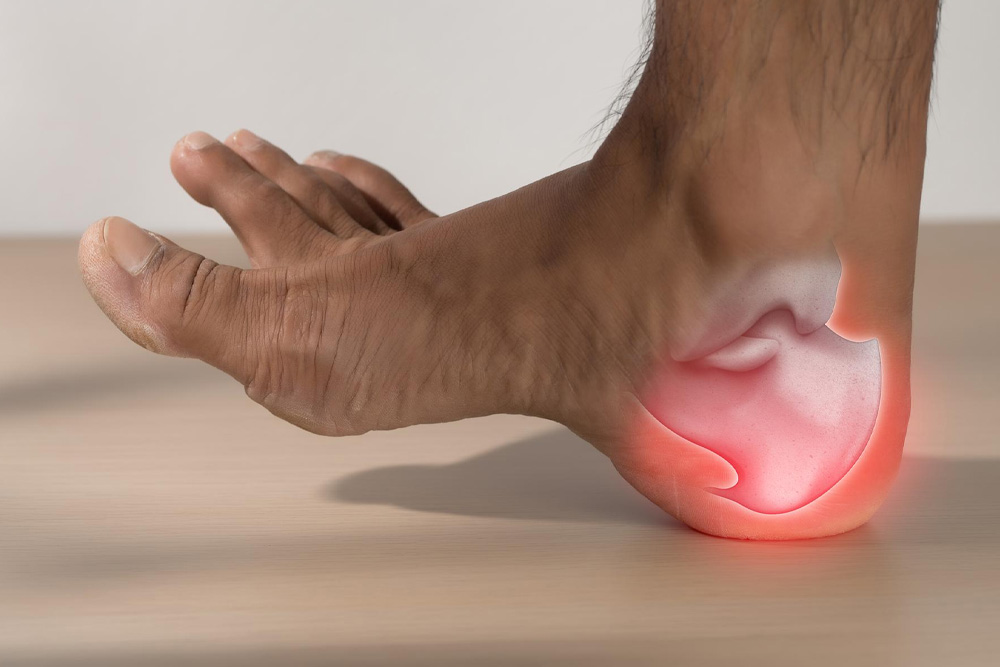
Flat feet occur when the arch of the foot collapses, causing the entire sole to make full contact with the ground when standing. Some people are born with flat feet; others develop them gradually with age, weight gain, or injury.
Not everyone with flat feet experiences pain. But when the arch collapses significantly, it can create abnormal stress throughout the foot, ankle, knee, and even the lower back.
Pain from flat feet typically occurs along the inner edge of the foot, in the arch, or in the heel. The feet may also tire easily after standing or walking for extended periods.
Treatment includes supportive footwear, custom orthotics, and physical therapy exercises to strengthen the foot muscles and improve alignment.
High Arches (Cavus Foot)
The opposite of flat feet, cavus foot describes a condition where the arch is abnormally high. This concentrates pressure on the heel and ball of the foot rather than distributing it evenly.
People with high arches are more prone to ankle sprains, stress fractures, and pain in the bottom of the foot. The foot may feel rigid and unstable, especially on uneven surfaces.
High arches can be inherited or caused by neurological conditions such as Charcot-Marie-Tooth disease, cerebral palsy, or the after-effects of a stroke.
Supportive footwear with cushioning, custom orthotics, and physical therapy are the primary treatments. In severe cases, surgery may be recommended to correct the arch alignment.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome occurs when the posterior tibial nerve — which runs through a narrow channel (the tarsal tunnel) on the inside of the ankle — becomes compressed. The pain radiates to the bottom of the foot, causing burning, tingling, or a shooting sensation.
It is the foot’s equivalent of carpal tunnel syndrome in the wrist. The condition can worsen with prolonged standing, walking, or activity.
Causes include flat feet that cause the nerve to stretch, ankle injuries, swelling from arthritis, or the presence of a cyst or other mass within the tarsal tunnel.
Treatment ranges from rest, orthotics, and anti-inflammatory medications to corticosteroid injections and, in more severe cases, surgical decompression of the tunnel.
Peripheral Neuropathy and Diabetes-Related Foot Pain
Peripheral neuropathy refers to nerve damage in the feet and lower legs. The bottom of the foot may feel numb, burning, or as though pins and needles are constantly present.
Diabetes is the leading cause of peripheral neuropathy. High blood sugar levels over time damage the small blood vessels that supply the nerves, leading to progressive nerve dysfunction.
The pain is often described as burning, electric shock-like, or extreme sensitivity to even light touch. Some people experience the opposite — complete numbness in the bottom of the foot.
People with diabetes must check their feet daily for cuts, sores, or blisters. Because nerve damage impairs sensation, injuries can go unnoticed and become serious infections. Early management of blood sugar levels is the most important preventive step.
Sesamoiditis
Sesamoids are two small bones embedded in the tendons beneath the big toe joint. They help absorb weight and movement during activities like walking, running, and bending the toe.
Sesamoiditis is inflammation of the tendons surrounding these bones. It is common in runners, ballet dancers, and people who spend long hours on the balls of their feet.
Pain is felt directly under the big toe joint at the front of the bottom of the foot. It worsens with activity and may be accompanied by swelling and bruising.
Treatment includes rest, padding inside the shoe, taping the toe, wearing low-heeled shoes, and anti-inflammatory medication. Steroid injections may be considered for stubborn cases.
Plantar Warts
Plantar warts are small growths caused by the human papillomavirus (HPV) that appear on the bottom of the foot, usually around the heel or ball. They often have a rough, grainy surface with tiny black dots (clotted blood vessels) visible inside.
Because they grow inward under the pressure of body weight, plantar warts can cause significant discomfort — especially when walking or standing.
They are contagious and spread through direct contact with the virus, often in communal areas like swimming pools, locker rooms, and public showers.
Over-the-counter salicylic acid treatments can remove plantar warts gradually. A podiatrist can also remove them using cryotherapy (freezing), laser treatment, or minor surgery.
Stone Bruise
A stone bruise is a deep bruise of the fat pad of the heel or ball of the foot, typically from stepping on a hard object like a rock or a sharp surface.
The pain is localized and feels like a persistent, tender ache directly under the point of impact. Unlike plantar fasciitis, the pain does not usually radiate to the arch.
Rest and cushioned footwear are the main treatments. Most stone bruises heal within a few days to weeks on their own with reduced weight-bearing activity.
Stress Fractures
Stress fractures are small cracks in the bones of the foot caused by repetitive force rather than a single traumatic injury. They are common in runners who suddenly increase their training volume, military recruits, and people with osteoporosis.
The metatarsal bones in the forefoot are the most frequently affected. Pain starts gradually and worsens with activity, usually improving with rest.
Swelling, tenderness directly over the bone, and pain that increases when you hop on the affected foot are key warning signs. A stress fracture requires medical evaluation — X-rays or an MRI scan are usually needed for diagnosis.
Treatment involves rest, a walking boot, and reduced weight-bearing activity for several weeks. Returning to activity too soon risks a complete fracture.
Gout
Gout is a form of inflammatory arthritis caused by the buildup of uric acid crystals in the joints. While it most commonly attacks the big toe joint, it can cause severe pain across the ball and bottom of the foot.
A gout attack comes on suddenly and without warning. The affected area becomes intensely painful, red, swollen, and warm to the touch — often overnight.
Diet plays a major role. Foods high in purines — red meat, shellfish, beer, and sugary drinks — raise uric acid levels and trigger attacks. Medications to reduce uric acid levels and manage inflammation are the standard treatment.
How to Treat Bottom of Foot Pain at Home
For most cases of bottom-of-foot pain, home treatment is the first and often most effective step. Here is what the evidence supports:
Rest: Reduce or stop activities that aggravate your foot. Give the inflamed tissues time to calm down.
Ice therapy: Apply an ice pack wrapped in a cloth to the painful area for 15–20 minutes, two to three times per day. Never apply ice directly to the skin.
Anti-inflammatory medication: Over-the-counter NSAIDs like ibuprofen (Advil, Motrin) reduce both pain and inflammation. Follow dosing instructions and consult your doctor if you have stomach or kidney concerns.
Supportive footwear: Wear shoes with adequate arch support and cushioning. Avoid walking barefoot, especially on hard floors. Flip-flops and flat shoes without support make most conditions worse.
Orthotics and insoles: Over-the-counter arch support insoles can significantly relieve plantar fasciitis and metatarsalgia. Custom orthotics from a podiatrist provide a more precise fit for chronic or structural issues.
Stretching: Daily stretching of the plantar fascia, calf muscles, and Achilles tendon is one of the most effective long-term treatments for bottom-of-foot pain.
Foot massage: Rolling a tennis ball or frozen water bottle under the arch of the foot for 5–10 minutes reduces tension and inflammation in the plantar fascia.
Elevation: Keeping your foot raised above heart level when resting reduces swelling and speeds up recovery.
Best Stretches for Bottom of Foot Pain
Stretching is a cornerstone of recovery for plantar fasciitis and arch pain. Do these exercises daily — especially first thing in the morning before your first steps.
Plantar Fascia Stretch
Sit in a chair. Cross one ankle over the opposite knee. Hold your toes and gently pull them back toward your shin until you feel a stretch along the arch. Hold for 15–30 seconds, repeat 3 times on each side.
Calf Stretch (Standing)
Stand an arm’s length from a wall with hands flat against it. Step one foot back and keep the heel flat on the ground. Bend the front knee and lean forward until you feel a stretch in the back calf. Hold for 30 seconds, repeat 3 times per side.
Towel Stretch
Sit with legs extended. Wrap a towel around the ball of your foot and gently pull it toward you, keeping the knee straight. Hold 30 seconds, repeat 3 times.
Toe Curl
Sit in a chair. Place a small towel flat on the floor. Use your toes to crumple and scrunch the towel toward you. This strengthens the intrinsic foot muscles that support the arch.
Frozen Water Bottle Roll
Freeze a water bottle and place it on the floor. Roll the bottom of your foot over it for 10 minutes. The cold reduces inflammation while the rolling massages and stretches the plantar fascia.
When to See a Doctor
Home treatment works well for most cases of bottom-of-foot pain — but there are clear signals that professional evaluation is needed.
| See a Doctor If… | Reason |
|---|---|
| Pain lasts more than 2 weeks without improvement | May need imaging or prescription treatment |
| Severe pain or sudden onset | Could indicate fracture or rupture |
| Foot pain after an injury or fall | Possible fracture or ligament damage |
| Redness, warmth, or swelling | Signs of infection or inflammatory condition |
| You have diabetes | Nerve damage masks injury — check immediately |
| You cannot bear weight on the foot | Structural damage likely |
| Numbness, tingling, or burning that spreads | Nerve compression or neuropathy |
A podiatrist (foot specialist) or orthopedic surgeon who specializes in foot and ankle conditions can provide a proper diagnosis through physical examination, gait analysis, and imaging studies such as X-rays or MRI scans.
Medical Treatments for Persistent Foot Pain
When home remedies are not enough, doctors have several effective options:
Physical therapy: A therapist designs a targeted program of stretches, strengthening exercises, and manual therapy to address the root mechanical cause of your foot pain.
Custom orthotics: Molded to the exact shape of your foot, custom insoles correct biomechanical problems that over-the-counter insoles cannot fix.
Corticosteroid injections: A direct injection of anti-inflammatory steroid medication into the painful area provides significant short-term relief for plantar fasciitis, metatarsalgia, and Morton’s neuroma.
Night splints: Worn during sleep, a night splint holds the foot in a dorsiflexed position, keeping the plantar fascia gently stretched overnight. Yale Medicine research shows this can bring relief within days for plantar fasciitis.
Walking boot: A short course of immobilization in a walking boot (2–6 weeks) removes stress from the plantar fascia while allowing some mobility.
Extracorporeal shockwave therapy (ESWT): A non-surgical procedure that uses sound waves to stimulate healing in chronic plantar fasciitis. It is often tried before surgery.
Surgery: Reserved for cases that do not respond to 6–12 months of conservative treatment. Plantar fascia release surgery cuts part of the plantar fascia to relieve tension. Most people improve significantly without reaching this stage.
How to Prevent Bottom of Foot Pain
Prevention is far easier than treatment. These habits protect the bottom of your foot from injury and chronic conditions:
Choose the right shoes. Look for a firm, supportive midsole and a deep heel cup. Avoid thin-soled shoes, high heels, and worn-out sneakers. Replace running shoes every 300–500 miles.
Stretch daily. Keep your calves, Achilles tendon, and plantar fascia flexible. Morning stretching before your first steps is especially important.
Maintain a healthy weight. Every pound of excess body weight puts approximately 3 pounds of force on the feet when walking. Even modest weight loss reduces foot pain significantly.
Increase activity gradually. Sudden spikes in running mileage or time on your feet are a leading cause of plantar fasciitis and stress fractures. Follow the 10% rule — do not increase weekly activity by more than 10% at a time.
Never walk barefoot on hard surfaces. Tile, concrete, and hardwood floors offer zero arch support. Wear supportive house shoes or slippers indoors.
Strengthen your feet. Exercises like toe curls, heel raises, and single-leg balance drills build the intrinsic muscles that support the arch and reduce injury risk.
Manage underlying conditions. If you have diabetes, control your blood sugar carefully. If you have arthritis, work with your doctor to keep inflammation under control.
Footwear Guide: What to Look for
The wrong shoes are one of the most preventable causes of bottom-of-foot pain. Here is what to look for:
| Feature | Why It Matters |
|---|---|
| Firm midsole | Supports the arch and absorbs shock |
| Deep heel cup | Holds the foot in proper alignment |
| Wide toe box | Prevents compression of metatarsals and toes |
| Cushioned insole | Protects the fatty heel pad and ball of foot |
| Low to moderate heel | Reduces pressure on the forefoot |
| Flexibility under ball of foot | Allows natural toe-off motion |
| Breathable upper | Reduces moisture and skin irritation |
Avoid shoes that bend easily in the middle, have no heel structure, or feel hard underfoot. These designs force your plantar fascia to work harder than it should.
If you spend long hours standing on hard floors, invest in an anti-fatigue mat. These foam or gel surfaces dramatically reduce stress on the bottom of the foot during prolonged standing.
The RICE Method for Foot Pain
For acute or sudden bottom-of-foot pain — especially after an injury — the RICE method is your first line of response.
Rest: Stop the activity immediately. Avoid putting weight on the foot.
Ice: Apply a wrapped ice pack for 15–20 minutes every 2–3 hours for the first 48 hours.
Compression: Wrap the foot snugly with an elastic bandage to reduce swelling. Do not wrap too tightly.
Elevation: Keep the foot raised above heart level as much as possible, including while sleeping.
Begin the RICE method within the first hour of injury for the best results. If pain is severe or you cannot bear weight, seek medical attention promptly.
Frequently Asked Questions (FAQs)
Why does the bottom of my foot hurt when I first wake up?
Morning pain is the classic sign of plantar fasciitis. The plantar fascia tightens overnight and stretches painfully with your first steps — it usually improves after a few minutes of walking.
Why does the bottom of my foot hurt when I walk?
Walking pain in the bottom of the foot is most commonly caused by plantar fasciitis, metatarsalgia, flat feet, or heel spurs — all of which worsen with repeated weight-bearing pressure.
Can bad shoes cause pain in the bottom of the foot?
Yes. Shoes with poor arch support, worn-out soles, or an overly narrow toe box are among the most common causes of plantar fasciitis, metatarsalgia, and chronic bottom-of-foot pain.
How long does bottom of foot pain take to heal?
Mild cases resolve in a few days to 2 weeks with rest and home care. Plantar fasciitis can take 6–18 months to fully recover, though most people feel significant improvement within 3 months of consistent treatment.
Should I walk on a painful foot or rest it?
Mild discomfort can tolerate gentle walking in supportive footwear. But sharp, severe, or worsening pain requires rest — continuing to walk on an injured foot prolongs healing and can cause further damage.
When should I see a podiatrist for bottom of foot pain?
See a podiatrist if pain lasts more than 2 weeks without improvement, if it is severe, if you cannot bear weight, or if you have diabetes, numbness, or signs of infection in the foot.
Can stretching actually fix bottom of foot pain?
Yes, stretching is one of the most evidence-backed treatments for plantar fasciitis and arch pain. Daily calf and plantar fascia stretches reduce tension on the heel and significantly speed up recovery.
Is it safe to run with pain in the bottom of my foot?
Running is not recommended during an active flare-up of plantar fasciitis, stress fractures, or metatarsalgia. Low-impact alternatives like swimming and cycling allow cardiovascular fitness to be maintained while the foot heals.
What is the fastest way to relieve pain in the bottom of the foot?
The fastest relief comes from combining rest, icing for 15–20 minutes, an OTC anti-inflammatory like ibuprofen, and wearing supportive footwear immediately. A frozen water bottle rolled under the arch also provides quick pain relief.
Can flat feet cause pain in the bottom of the foot?
Yes. Flat feet alter the mechanics of the entire foot, placing abnormal stress on the plantar fascia, heel, and surrounding tissues. Supportive orthotics and arch-support shoes are the most effective management strategy.
Conclusion
Why does the bottom of my foot hurt is a question with many possible answers — from plantar fasciitis and heel spurs to metatarsalgia, nerve damage, and structural foot problems.
The key is identifying where on the bottom of the foot the pain is located and understanding what symptoms accompany it.
Most cases respond well to rest, ice, proper footwear, daily stretching, and over-the-counter orthotics. Start treatment early rather than pushing through the pain — delay makes most conditions harder to resolve.
If pain persists beyond two weeks, worsens, or is accompanied by swelling, numbness, or an inability to bear weight, see a podiatrist or orthopedic specialist.
With the right diagnosis and a consistent treatment plan, the vast majority of people fully recover and return to pain-free daily life within a few months.