Why am I suddenly lactose intolerant is a question millions of adults ask every year after noticing that dairy foods they once enjoyed now cause painful bloating, gas, and cramps.
This can feel confusing and alarming, especially when you have eaten dairy your entire life without a single problem.
The truth is, sudden lactose intolerance is far more common than most people realize. It can develop at any age, often without warning.
Fortunately, the causes are well understood, the condition is manageable, and you do not have to give up dairy forever.
What Is Lactose Intolerance and Why Does It Happen
Lactose intolerance is not a food allergy. It is a digestive issue caused by the body not producing enough lactase — the enzyme responsible for breaking down lactose, the natural sugar found in milk and dairy products.
When lactase levels drop too low, undigested lactose passes into the colon. Bacteria in the colon then begin to ferment that undigested sugar, releasing gas, acids, and fluids that trigger uncomfortable symptoms.
The process is automatic and not dangerous, but it can cause significant discomfort within 30 minutes to 2 hours of eating dairy.
How Common Is Sudden Lactose Intolerance
Sudden lactose intolerance is far more widespread than most people expect. According to research, up to 68% of the global population has some degree of difficulty digesting lactose.
Primary lactase deficiency — the most common form — typically becomes noticeable by the age of 20, though symptoms can first appear in the 30s, 40s, or even later in life.
The condition does not discriminate by age. Adults who have tolerated dairy for decades can begin developing symptoms seemingly overnight.
The Science Behind Lactase Decline
The human body naturally produces less lactase as it ages. This decline begins in infancy after breastfeeding ends and continues gradually across a person’s entire lifetime.
The LCT gene controls lactase production. When this gene “switches off,” lactase output slows dramatically. Some people inherit a version of the gene that keeps production going well into adulthood, while others see a steep drop in their 20s or 30s.
Symptoms typically only begin once lactase levels fall below roughly 50% of what the body needs to digest a standard dairy portion. Up until that point, many people have no idea the decline is even happening.
Why Am I Suddenly Lactose Intolerant — The Main Causes
There is rarely just one reason why lactose intolerance develops suddenly. Below are the most common causes identified by gastroenterologists and digestive health researchers.
1. Natural Aging and Lactase Decline
The most frequent reason adults develop sudden dairy intolerance is simply age. As the body grows older, the small intestine produces progressively less lactase.
This process is gradual, but the tipping point — where symptoms finally appear — can feel sudden. One day dairy is fine; the next it causes bloating and cramps.
This is known as primary lactose intolerance or lactase nonpersistence, and it accounts for the vast majority of adult-onset cases worldwide.
2. Gut Infection or Stomach Bug
A gastrointestinal infection can damage the lining of the small intestine and temporarily reduce lactase production. This is called secondary lactose intolerance.
Common culprits include bacterial infections like Salmonella or E. coli, viral gastroenteritis (stomach flu), and parasitic infections such as Giardia.
In many cases, lactase levels recover once the infection clears — meaning the intolerance may be temporary. However, recovery can take weeks to months depending on the severity of the damage.
3. Celiac Disease
Celiac disease is an autoimmune condition triggered by gluten. When a person with undiagnosed celiac continues eating gluten, the immune system attacks the villi — tiny finger-like projections in the small intestine that produce digestive enzymes including lactase.
Damage to the villi directly reduces lactase production, which is why many people with undiagnosed celiac develop sudden dairy intolerance before receiving their celiac diagnosis.
Treating celiac with a strict gluten-free diet often allows the intestinal villi to heal and lactase levels to partially or fully recover over time.
4. Crohn’s Disease and Inflammatory Bowel Disease
Crohn’s disease causes chronic inflammation in the digestive tract, most often in the small intestine. This ongoing inflammation can directly impair lactase production and reduce the gut’s ability to absorb lactose.
Individuals with Crohn’s or other forms of inflammatory bowel disease are significantly more likely to develop lactose intolerance compared to the general population.
Managing the underlying IBD through medication and dietary changes is the most effective strategy for improving dairy tolerance in these cases.
5. Small Intestinal Bacterial Overgrowth (SIBO)
SIBO occurs when an abnormal amount of bacteria colonizes the small intestine — an area that should have relatively low bacterial counts. These bacteria interfere with digestion and can rapidly ferment lactose before the body has a chance to absorb it.
The result is bloating, gas, diarrhea, and cramping that closely mimics classic lactose intolerance. In fact, SIBO is frequently misdiagnosed as lactose intolerance, and vice versa.
A hydrogen breath test can help distinguish between the two conditions. Treating SIBO with targeted antibiotics or dietary protocols often resolves the apparent dairy sensitivity.
6. Prolonged Dairy Abstinence
If you have avoided dairy for an extended period — whether for dietary, ethical, or health reasons — your gut may have reduced the amount of lactase it produces because it was not being regularly triggered.
The body is highly adaptive. When lactase is not in demand for weeks or months, production can scale down. Reintroducing dairy suddenly after a long break can feel like developing a new intolerance.
The good news is that gradual reintroduction of small dairy portions can help retrain the gut to produce more lactase again over time.
7. Cancer Treatment — Radiation and Chemotherapy
Radiation therapy directed at the abdominal or pelvic region can damage the small intestine and severely reduce lactase production. This is a well-documented side effect of cancer treatment.
Chemotherapy can also cause intestinal inflammation and disruption that impairs normal digestive enzyme activity, including lactase.
In some cases, lactase levels may partially recover after treatment ends, but for others the lactose intolerance becomes permanent.
8. Gastrointestinal Surgery
Any surgery involving the small intestine — including bowel resection, gastric bypass, or procedures for Crohn’s disease — can reduce the surface area available for lactase production.
Less functional intestinal lining means less lactase, which means less ability to digest lactose. People who have undergone GI surgeries should discuss dairy tolerance with their gastroenterologist as part of post-surgical dietary planning.
9. Genetics and Ethnicity
Genetics plays a significant role in determining both when lactose intolerance develops and how severe it becomes. Lactase nonpersistence has a strong hereditary component and varies significantly by ancestral background.
Lactose intolerance is more prevalent among people of East Asian, West African, Arab, Greek, Italian, Jewish, Hispanic, and Native American descent compared to those of Northern European ancestry, where lactase persistence is more common.
If your parents or siblings are lactose intolerant, your risk of developing sudden dairy intolerance as an adult is higher than average.
10. Irritable Bowel Syndrome (IBS)
IBS is a chronic gut condition characterized by abdominal pain, bloating, constipation, and diarrhea. Many people with IBS also have heightened sensitivity to certain foods — including dairy — regardless of whether their lactase levels are technically low.
The overlap between IBS symptoms and lactose intolerance symptoms can make diagnosis tricky. Keeping a detailed food diary is one of the most reliable first steps in identifying whether dairy specifically is the trigger.
Lactose Intolerance vs Milk Allergy — Key Differences
Many people confuse lactose intolerance with a milk allergy, but they are completely different conditions with different causes and treatments.
| Feature | Lactose Intolerance | Milk Allergy |
|---|---|---|
| Cause | Enzyme deficiency (lactase) | Immune system reaction to milk protein |
| System Affected | Digestive system | Immune system |
| Symptoms | Bloating, gas, cramps, diarrhea | Hives, wheezing, anaphylaxis, rash |
| Age of Onset | Any age, most common in adults | Usually appears in infancy |
| Life-Threatening? | No | Can be (anaphylaxis) |
| Treated By | Diet, enzyme supplements | Complete dairy avoidance |
Understanding the difference matters. A milk allergy requires strict elimination of all dairy. Lactose intolerance can often be managed with partial dairy reduction and enzyme support.
Types of Lactose Intolerance Explained
There are four recognized types of lactose intolerance, each with a different cause and prognosis.
| Type | Cause | Reversible? |
|---|---|---|
| Primary (Lactase Nonpersistence) | Genetic decline in lactase with age | No, but manageable |
| Secondary | Illness, infection, surgery, or injury | Often yes, with treatment |
| Congenital | Rare genetic condition from birth | No |
| Developmental | Premature birth (temporary) | Usually yes, as infant matures |
Most adults who develop sudden lactose intolerance fall into either the primary or secondary category. Secondary cases have the best chance of full or partial recovery once the underlying cause is treated.
Common Symptoms of Sudden Lactose Intolerance
Recognizing the symptoms is the first step toward getting help. Symptoms typically appear within 30 minutes to 2 hours after consuming dairy.
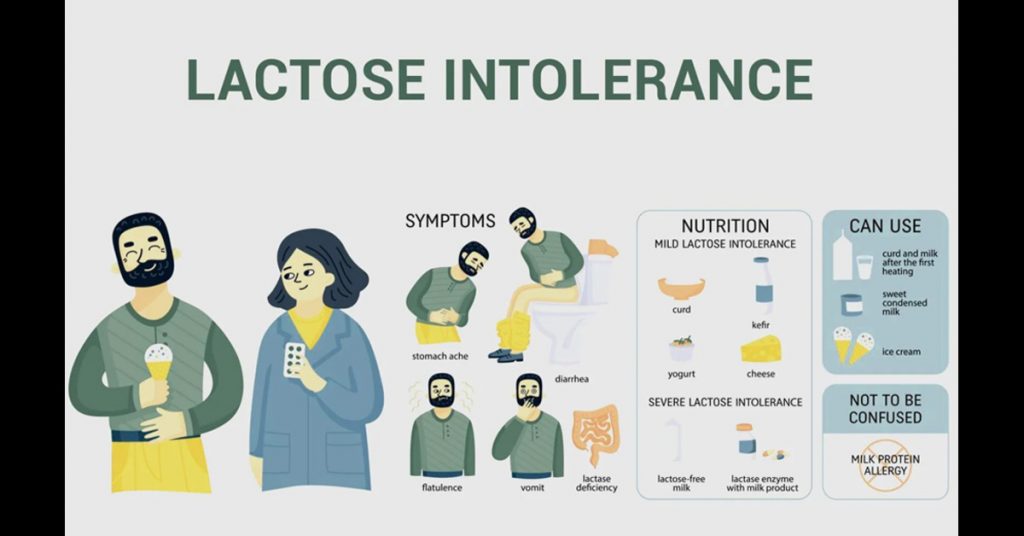
The most common symptoms include bloating and abdominal distension, gas and flatulence, stomach cramps and abdominal pain, diarrhea, nausea, and in some cases vomiting. Symptom severity depends on how much lactose was consumed, how low your lactase levels are, and individual gut sensitivity.
Some people can tolerate small amounts of dairy with no symptoms, while others react strongly to even a small splash of milk in coffee.
Foods That Contain Hidden Lactose
Lactose is not only found in obvious dairy products. It is also added to many processed and packaged foods, which can make symptoms harder to trace.
| High Lactose Foods | Moderate Lactose Foods | Low Lactose Foods |
|---|---|---|
| Regular milk | Ice cream | Hard aged cheeses (cheddar, parmesan) |
| Soft cheeses (ricotta, cottage) | Sour cream | Butter |
| Cream soups | Cream cheese | Greek yogurt |
| Milk chocolate | Milk-based protein shakes | Lactose-free milk |
| Puddings and custards | Pancake mixes | Probiotic yogurt |
Hidden lactose also appears in bread and baked goods, instant mashed potatoes, breakfast cereals, salad dressings, some medications and antacids, chocolate candies, and non-dairy creamers. Always read ingredient labels and look for words like milk, whey, milk solids, dry milk powder, and curds.
How to Test for Lactose Intolerance

If you suspect you are suddenly lactose intolerant, there are several ways to confirm the diagnosis.
A hydrogen breath test is the most widely used diagnostic method. You consume a measured dose of lactose and then breathe into a device at regular intervals. Elevated hydrogen and methane levels indicate that lactose is fermenting in your colon rather than being absorbed.
A lactose tolerance blood test measures blood glucose levels after a lactose drink. If glucose does not rise, it means your body is not digesting and absorbing the lactose properly.
A stool acidity test is primarily used for infants and young children. It detects lactic acid and other acids produced when lactose ferments in the colon.
A food and symptom diary is a practical first step you can do at home. Record everything you eat and drink alongside any symptoms that follow over 5 to 7 days. A clear pattern linking dairy consumption to GI symptoms is a strong indicator.
An elimination diet involves removing all dairy for 2 to 4 weeks and then reintroducing it systematically. If symptoms disappear during elimination and return when dairy is reintroduced, lactose intolerance is the likely cause.
10 Proven Fixes for Sudden Lactose Intolerance
The good news is that sudden lactose intolerance does not mean you have to completely give up dairy for life. There are many effective management strategies available.
Fix 1 — Take Lactase Enzyme Supplements
Over-the-counter lactase supplements (such as Lactaid) are among the most effective short-term solutions. You take one with your first bite of dairy, and the supplement provides the enzyme your body is not producing in sufficient quantities.
They are widely available at pharmacies and supermarkets without a prescription. They work best when taken consistently before dairy consumption rather than after symptoms start.
Fix 2 — Start with Small Amounts of Dairy
Consuming small portions of dairy — rather than large amounts at once — reduces the lactose load on your digestive system. Your gut can often handle trace amounts even when full portions cause problems.
Begin with a tablespoon of milk in coffee and gradually increase over several weeks. Many people can retrain their gut to tolerate more lactose through this gradual exposure technique.
Fix 3 — Eat Dairy with Other Foods
Consuming dairy alongside other foods — especially those high in fat or fiber — slows gastric emptying and gives your remaining lactase more time to break down lactose before it reaches the colon.
Try having cheese with crackers, milk with cereal, or yogurt mixed into a meal. Eating dairy on an empty stomach dramatically increases the likelihood of symptoms.
Fix 4 — Choose Lower-Lactose Dairy Products
Not all dairy products contain the same amount of lactose. Hard aged cheeses like cheddar, parmesan, and Swiss have very low lactose levels because the aging process causes bacteria to consume most of the lactose.
Greek yogurt and probiotic yogurts with live active cultures are also generally better tolerated because the bacteria help digest lactose. Butter and ghee contain minimal lactose and are usually safe for most lactose-intolerant individuals.
Fix 5 — Switch to Lactose-Free Dairy
Lactose-free versions of milk, cheese, ice cream, and yogurt are now widely available and taste virtually identical to regular dairy. These products have lactase pre-added so the lactose is already broken down before you consume it.
Lactose-free milk contains the same calcium, protein, and vitamin D as regular milk, making it an excellent nutritional swap with zero digestive downside.
Fix 6 — Try Plant-Based Dairy Alternatives
A wide range of plant-based milks are now available that contain zero lactose. Popular options include oat milk, almond milk, soy milk, coconut milk, rice milk, and hemp milk.
Soy milk is generally the closest nutritional match to cow’s milk, especially for protein content. Many plant-based milks are also fortified with calcium and vitamin D to help you maintain adequate nutrient levels.
Fix 7 — Add Probiotics to Your Diet
Probiotics — beneficial bacteria found in foods like yogurt, kefir, sauerkraut, and kimchi — can improve gut health and may help reduce lactose intolerance symptoms over time.
Research has found that certain strains of lactic acid bacteria help convert lactose into lactic acid rather than gas, reducing fermentation and the discomfort that follows. Regular probiotic use supports the overall microbiome balance in the colon.
Fix 8 — Treat the Underlying Condition
If your sudden lactose intolerance is secondary — caused by celiac disease, SIBO, Crohn’s, or another gut condition — treating that underlying problem is the most important step.
In many secondary cases, lactase levels partially or fully recover once the root cause is properly managed. Work with a gastroenterologist to identify and treat any underlying digestive condition driving your new dairy sensitivity.
Fix 9 — Protect Your Calcium and Vitamin D Intake
One of the most important concerns with lactose intolerance is ensuring you still get enough calcium and vitamin D, both of which are abundant in dairy.
Non-dairy calcium sources include canned sardines and salmon (with bones), tofu, kale, broccoli, collard greens, dried beans, almonds, blackstrap molasses, and calcium-fortified orange juice. Vitamin D can be obtained from sunlight exposure and supplementation.
Talk to a registered dietitian to ensure your new dairy-reduced diet meets your nutritional needs, especially if you are an older adult or have bone health concerns.
Fix 10 — Keep a Food Diary and Track Your Threshold
Every person with lactose intolerance has a unique tolerance threshold — the amount of dairy they can consume before symptoms appear. Understanding your personal threshold is key to managing the condition without unnecessary restrictions.
Keep a food diary for at least one week, noting every dairy product, the portion size, and any symptoms that follow. Over time, you will identify which dairy products you can tolerate, in what amounts, and under what circumstances.
Lactose Content of Common Dairy Foods

Understanding which foods contain the most lactose helps you make smarter choices and avoid triggering symptoms unnecessarily.
| Food | Serving Size | Approximate Lactose Content |
|---|---|---|
| Whole milk | 1 cup (240ml) | 11-12g |
| Skim milk | 1 cup (240ml) | 12-13g |
| Ice cream | ½ cup | 6-7g |
| Soft cheese (ricotta) | ½ cup | 6-7g |
| Yogurt (regular) | 1 cup | 5-8g |
| Greek yogurt | 1 cup | 3-4g |
| Cheddar cheese (aged) | 1 oz | Less than 1g |
| Butter | 1 tbsp | Less than 0.5g |
| Lactose-free milk | 1 cup | 0g |
Most adults with lactose intolerance can tolerate up to 12g of lactose at one time — roughly equivalent to a single cup of milk. Spreading smaller amounts across the day is more manageable than consuming one large dairy portion.
When to See a Doctor
Sudden lactose intolerance usually has an identifiable, manageable cause. But certain symptoms alongside dairy-related discomfort warrant a medical evaluation.
See a doctor if you experience unexplained weight loss alongside GI symptoms, blood in your stool, persistent or severe abdominal pain that does not resolve, nausea or vomiting that is not linked to a specific meal, or diarrhea that lasts more than two weeks despite eliminating dairy.
These symptoms may point to conditions beyond simple lactose intolerance — including celiac disease, inflammatory bowel disease, or in rare cases colorectal concerns — that require professional investigation and treatment.
Lactose Intolerance and Bone Health
A long-term concern for people who reduce dairy intake is maintaining adequate bone density. Dairy is one of the most concentrated dietary sources of calcium, which is essential for bone strength throughout life.
Adults over 50 who develop lactose intolerance need to be especially careful. The risk of osteoporosis and bone fractures increases when calcium intake falls below recommended levels, and studies suggest that chronic dairy avoidance without nutritional compensation can accelerate bone mineral loss.
Prioritize calcium-rich non-dairy foods, consider a calcium supplement if dietary intake is insufficient, and discuss bone health monitoring with your healthcare provider if you have been lactose intolerant for more than a year.
The Role of the Gut Microbiome
Emerging research suggests that the gut microbiome — the community of bacteria living in your digestive tract — plays a role in how the body responds to lactose.
People with a richer, more diverse gut microbiome tend to experience less severe lactose intolerance symptoms, even with similar lactase enzyme levels. Regular lactose consumption in small amounts may actually function as a prebiotic, feeding beneficial gut bacteria like Bifidobacteria and Lactobacillus.
This means that avoiding dairy entirely may over time reduce the microbiome’s tolerance for lactose, making symptoms worse when you do consume it. Gradual, consistent small dairy portions may be more beneficial for long-term gut health than complete elimination.
Can Sudden Lactose Intolerance Go Away
Whether lactose intolerance is permanent depends largely on its cause. Primary lactose intolerance — the natural age-related decline in lactase — does not reverse. However, it can be effectively managed with the strategies described above.
Secondary lactose intolerance caused by an infection, celiac disease, or SIBO has a much better prognosis. Once the underlying gut condition heals, lactase levels can recover — sometimes fully — and dairy tolerance may return.
Even in cases where full recovery is not possible, most people find that their individual tolerance threshold is higher than they initially feared. With careful management, the majority of lactose-intolerant adults can continue enjoying some dairy without significant symptoms.
Sudden Lactose Intolerance During and After Pregnancy
Some women notice new or worsening dairy intolerance during pregnancy or shortly after giving birth. Hormonal changes during pregnancy can affect digestive motility and gut enzyme activity, sometimes triggering symptoms that were not present before.
Postpartum gut health changes — including shifts in the microbiome — can also influence lactose tolerance. In many cases, dairy sensitivity that develops during pregnancy improves in the months after delivery as gut health stabilizes.
Pregnant and breastfeeding women should discuss any significant dietary restrictions with a healthcare provider to ensure both mother and baby receive adequate calcium and other critical nutrients.
Building a Lactose-Friendly Diet Plan
Managing lactose intolerance does not mean a joyless, dairy-free life. With thoughtful planning, most people can maintain an enjoyable and nutritionally complete diet.
A practical starting point is to identify your personal threshold, then rebuild your diet around dairy portions that stay within that threshold. Add one or two lactase supplements per week for occasions when you want a larger dairy portion.
Include probiotic-rich foods like Greek yogurt, kefir, and fermented cheeses regularly to support gut health. Fill any calcium gaps with leafy greens, fortified plant-based milks, beans, and fish with edible bones. Recheck your tolerance every few months, as it can shift — sometimes improving — with consistent gut support.
Frequently Asked Questions (FAQs)
Why am I suddenly lactose intolerant when I never was before?
Lactase production naturally declines with age, and a tipping point can be reached at any time in adulthood. A recent gut infection, illness, or digestive condition can also trigger sudden onset.
Can you develop lactose intolerance in your 30s, 40s, or 50s?
Yes, completely. Most cases of primary lactose intolerance first appear between the ages of 20 and 50, though new onset at any adult age is common and normal.
Is sudden lactose intolerance permanent?
It depends on the cause. Primary age-related intolerance is not reversible, but secondary intolerance caused by infection or illness often resolves once the underlying issue heals.
What is the fastest fix for lactose intolerance symptoms?
Over-the-counter lactase enzyme supplements taken before eating dairy are the fastest and most reliable fix for preventing or reducing symptoms in the short term.
Can you reverse lactose intolerance naturally?
You cannot reverse primary lactose intolerance, but gradual reintroduction of small dairy portions, probiotic support, and treating underlying gut conditions can significantly improve tolerance over time.
Does lactose intolerance get worse with age?
For most people with primary lactase nonpersistence, symptoms can become more pronounced with age as lactase levels continue declining. Managing portion sizes becomes more important over time.
What dairy products can I still eat if I am lactose intolerant?
Hard aged cheeses like cheddar and parmesan, Greek yogurt, probiotic yogurt, butter, and lactose-free dairy products are typically well tolerated by most people with lactose intolerance.
Is lactose intolerance the same as a dairy allergy?
No. A dairy allergy is an immune system response to milk proteins and can be life-threatening. Lactose intolerance is a digestive enzyme deficiency that causes discomfort but is not dangerous.
How do I know if I have lactose intolerance or IBS?
A hydrogen breath test, elimination diet, and food diary can help distinguish the two. If symptoms occur specifically after dairy and improve when dairy is removed, lactose intolerance is the likely cause.
Can I get enough calcium without dairy if I am lactose intolerant?
Yes. Non-dairy calcium sources include kale, broccoli, tofu, canned sardines, almonds, fortified plant-based milks, and dried beans. A calcium supplement can also fill any dietary gaps.
Conclusion
Why am I suddenly lactose intolerant is a question with a clear and manageable answer in the vast majority of cases.
The most common reason is the natural age-related decline in lactase enzyme production — a process that affects up to 68% of people worldwide at some point in their lives.
Secondary causes like gut infections, celiac disease, SIBO, Crohn’s disease, cancer treatment, and prolonged dairy avoidance can also trigger sudden onset at any age.
The important thing to understand is that sudden lactose intolerance is not dangerous, not your fault, and in many cases partially or fully reversible.
With the right combination of dietary adjustments, lactase supplements, probiotic support, and medical treatment for any underlying condition, most people can continue enjoying dairy in some form.
Always consult a healthcare provider or gastroenterologist if symptoms are severe, persistent, or accompanied by warning signs that suggest a more serious underlying condition.

