Why is my gum swollen around one tooth in the back is one of the most common dental concerns people search for in 2026.
That sudden puffiness, tenderness, or throbbing around a single back tooth is your body telling you something is wrong.
It can range from a minor irritant like trapped food to a serious infection that needs urgent dental care.
What Does It Mean When Your Gum Is Swollen Around One Back Tooth
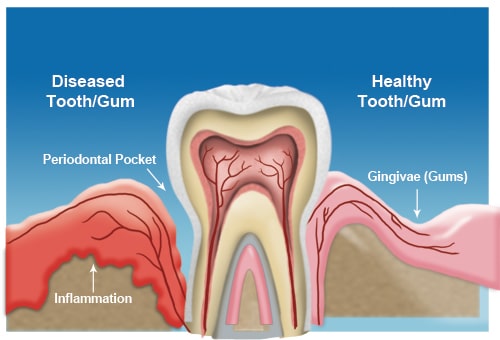
Swelling that appears around just one tooth — especially in the back of your mouth — almost always points to a localized problem. It is different from general gum inflammation that affects the whole mouth.
The back teeth, your molars and premolars, are harder to clean. Plaque and bacteria build up there faster. That makes the gum tissue around them more vulnerable to infection, injury, and disease.
When the gum tissue becomes inflamed, it swells as part of your body’s immune response. That swelling is a signal, not just a symptom. It means something in that specific area needs attention right away.
Why Back Teeth Are More Vulnerable to Gum Swelling
The position of back teeth makes them naturally harder to reach during daily brushing and flossing. Most people rush through cleaning their molars, leaving behind food debris and bacterial plaque.
Back teeth also have deep grooves and multiple roots. Bacteria can hide in those spaces and irritate the surrounding gum tissue for weeks before visible swelling appears.
In 2026, dental research continues to confirm that back molar gum swelling accounts for the majority of localized periodontal complaints seen in dental offices. The condition is extremely common — and very treatable when caught early.
Top Causes of Swollen Gum Around One Tooth in the Back
Understanding what is causing the swelling is the first step toward the right treatment. Here are the most common causes identified by dental professionals.
1. Trapped Food or Debris Under the Gumline
Food particles — especially popcorn husks, seeds, meat fibers, and small bone fragments — can lodge between a back tooth and the gum. Once stuck, they create a pocket of irritation that swells quickly.
The gum tissue responds by becoming inflamed within hours. The area may feel tender, look red, and occasionally produce a slight bad taste or odor.
This is the easiest cause to resolve. Careful flossing and a warm saltwater rinse often remove the debris and reduce swelling within one to two days.
2. Gingivitis — Early Stage Gum Disease
Gingivitis is the most common cause of swollen gum around one tooth in the back. It occurs when plaque — a sticky film of bacteria — builds up along the gumline and is not fully removed.
The bacteria in plaque irritate the gum tissue and trigger inflammation. The gum becomes red, puffy, and may bleed when you brush or floss.
Gingivitis is fully reversible with proper cleaning and improved oral hygiene. Left untreated, however, it progresses into a much more serious condition called periodontitis.
3. Periodontitis — Advanced Gum Disease
Periodontitis develops when gingivitis is ignored and the bacterial infection spreads deeper into the gum tissue, bone, and ligaments supporting the tooth. According to the Centers for Disease Control and Prevention, nearly 47 percent of adults over age 30 in the United States have some form of periodontal disease.
When periodontitis targets one specific back tooth, it creates a deep pocket between the gum and the tooth root. Bacteria accumulate in that pocket, causing significant swelling, bone loss, and eventually tooth loosening.
Periodontitis cannot be reversed — but it can be managed and stopped from progressing with professional dental treatment.
4. Dental Abscess — Infection and Pus Formation
A dental abscess is a pocket of pus caused by a serious bacterial infection. It is one of the most painful and urgent causes of swollen gum around one tooth in the back.
There are two main types. A periapical abscess forms at the tip of the tooth root, usually from untreated tooth decay or a cracked tooth. A periodontal abscess forms in the gum tissue next to the tooth, typically from advanced gum disease.
Both types cause intense, throbbing pain, visible swelling, bad breath, and sometimes fever. If you suspect an abscess, see a dentist immediately. The infection can spread to the jaw, neck, and beyond if left untreated.
5. Cracked or Fractured Tooth
A cracked tooth is a sneaky cause of localized gum swelling. Cracks can occur from chewing hard candy, grinding teeth at night, biting ice, or a sudden impact.
When a tooth cracks, bacteria enter the inner pulp through the fracture. This triggers infection and inflammation in both the tooth and the surrounding gum tissue. The swelling often appears directly next to the cracked tooth.
The problem is that cracks are often invisible to the naked eye. Only a dental X-ray or specific examination under bright light can confirm the fracture.
6. Impacted or Erupting Wisdom Tooth — Pericoronitis
If your swollen gum is specifically at the very back of your mouth, around your last molar, an impacted or partially erupted wisdom tooth is a highly likely cause.
When a wisdom tooth does not have enough room to fully emerge, it becomes partially trapped in the gum. A flap of gum tissue — called an operculum — covers part of the tooth. Food and bacteria get trapped underneath that flap, causing a painful condition called pericoronitis.
Pericoronitis symptoms include severe pain at the back of the mouth, swollen gum tissue, bad taste, difficulty swallowing, and in serious cases, jaw stiffness and facial swelling. It most commonly affects people aged 20 to 29.
7. Tooth Decay Reaching the Pulp
As a cavity progresses deeper into a tooth, it eventually reaches the pulp — the soft inner tissue containing nerves and blood vessels. Once bacteria infect the pulp, the surrounding gum tissue reacts with visible swelling.
This type of swelling is usually accompanied by sharp, intense tooth pain, especially when biting or drinking something hot or cold. A root canal is typically needed to remove the infected pulp and stop the swelling.
8. Gum Abscess After Dental Work
Swelling can occasionally appear after a recent dental procedure like a filling, crown placement, or extraction. Some post-procedure swelling is normal and expected.
However, if the swelling increases after 48 hours, is accompanied by fever, or produces pus, it may indicate infection at the treatment site. Contact your dentist immediately if this happens.
9. Trauma or Physical Injury to the Gum
A blow to the mouth, accidental bite on something hard, or overly aggressive brushing can bruise or tear the gum tissue around a back tooth. The injured tissue swells as it tries to heal.
Trauma-related swelling is usually temporary. It reduces within a few days with gentle care. If the swelling does not go down or worsens, a dentist should evaluate the area for hidden damage.
10. Hormonal Changes
Hormonal fluctuations during pregnancy, puberty, menstruation, or menopause can make gum tissue more sensitive and prone to swelling. This condition is sometimes called pregnancy gingivitis when it occurs during pregnancy.
Hormonal gum swelling can target specific teeth, especially if there is existing plaque buildup in that area. It does not mean permanent gum disease — but it does require careful monitoring and good oral hygiene.
Symptoms That Accompany Swollen Gum Around One Back Tooth
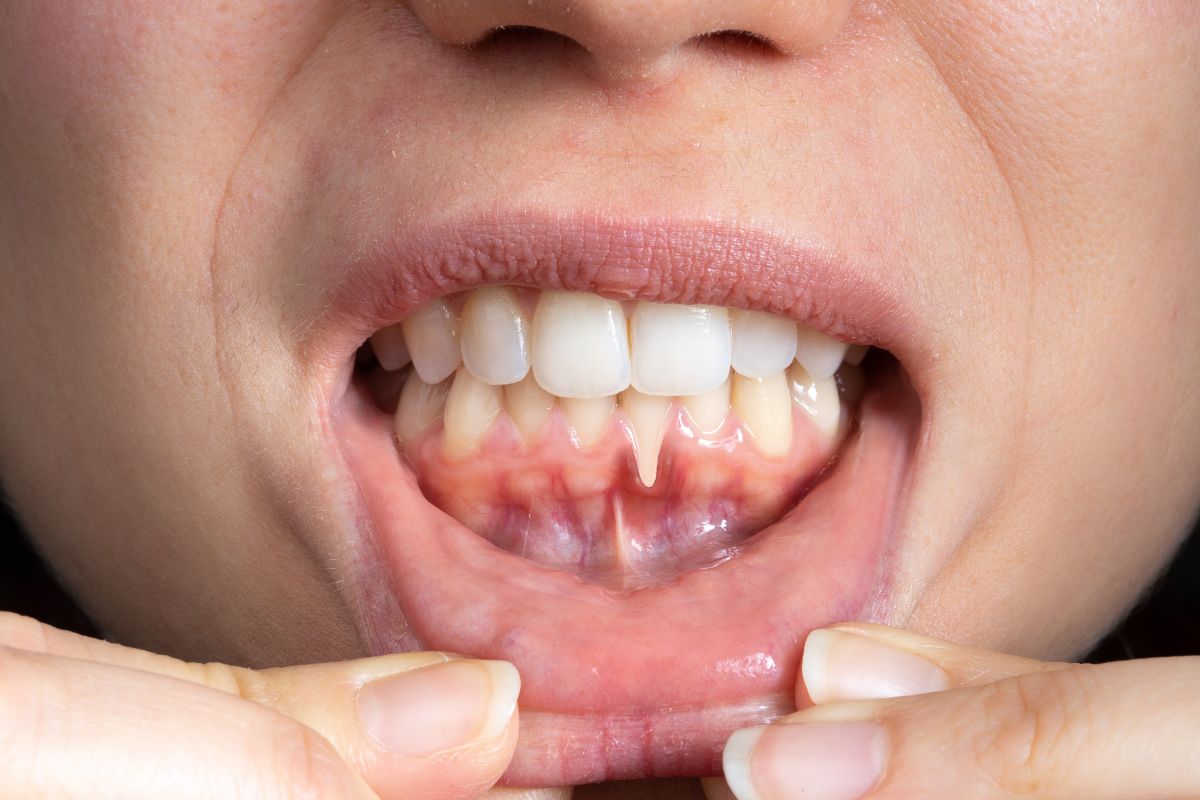
Recognizing all the symptoms helps you understand the severity of the problem and whether you need immediate dental care.
| Symptom | Possible Cause |
|---|---|
| Throbbing, pulsing pain | Dental abscess or deep infection |
| Bleeding when brushing | Gingivitis or periodontitis |
| Pus or discharge | Abscess — seek urgent dental care |
| Bad taste or bad breath | Trapped debris, abscess, or infection |
| Swelling that spreads to cheek | Spreading infection — go immediately |
| Loose-feeling tooth | Advanced periodontitis or abscess |
| Fever with swelling | Serious infection — urgent care needed |
| Pain spreading to jaw or ear | Pericoronitis or deep abscess |
| White or pale gum tissue | Localized infection or bacterial reaction |
| Sensitivity to hot and cold | Decay reaching pulp or cracked tooth |
Never ignore fever, spreading swelling, difficulty swallowing, or pus. These are signs of a serious infection that can become life-threatening if it spreads beyond the jaw.
How to Diagnose the Cause of Gum Swelling Around One Back Tooth
Your dentist will begin with a thorough visual examination of the swollen gum and surrounding tooth. They will probe the gum pocket depth using a small instrument to check for signs of periodontitis.
Dental X-rays are almost always taken to check for bone loss, abscesses at the root tip, cracks in the tooth, or impacted wisdom teeth. These images reveal what cannot be seen with the naked eye.
In some cases, a dentist may also check bite alignment, look for craze lines or fractures under special lighting, and review your full medical and dental history for contributing factors.
Professional Treatment Options for Swollen Gum Behind Back Tooth
Treatment depends entirely on what is causing the swelling. Here is a clear breakdown of the most common dental treatments used in 2026.
| Cause | Professional Treatment |
|---|---|
| Trapped food / mild irritation | Professional cleaning + hygiene guidance |
| Gingivitis | Scaling, polishing, oral hygiene instruction |
| Periodontitis | Scaling and root planing (deep cleaning) |
| Dental abscess | Drainage, root canal or extraction, antibiotics |
| Cracked tooth | Crown, root canal, or extraction depending on severity |
| Pericoronitis | Irrigation, antibiotics, operculum removal, wisdom tooth extraction |
| Pulp infection from decay | Root canal therapy |
| Post-procedure infection | Antibiotics, irrigation, possible re-treatment |
Scaling and Root Planing — Deep Cleaning
This is the standard treatment for gum disease-related swelling. The dentist or hygienist uses specialized instruments to remove plaque and tartar from both above and below the gumline.
Root planing smooths the root surface, making it harder for bacteria to reattach. Local anesthesia is used so the procedure is comfortable. Most patients see significant improvement within one to two weeks.
Root Canal Therapy
When the cause of gum swelling is a pulp infection or abscess originating inside the tooth, a root canal removes the infected tissue. The tooth is cleaned, shaped, filled, and sealed.
Root canals save the natural tooth and eliminate the source of infection. Gum swelling typically begins to reduce within days of the procedure as the infection is removed.
Abscess Drainage
If a visible pocket of pus has formed in the gum, the dentist will make a small incision to drain it. This immediately relieves pressure and pain. Antibiotics are prescribed to eliminate the remaining bacteria.
Drainage alone does not cure the underlying problem. A root canal or extraction is usually required to address the original source of the infection.
Wisdom Tooth Extraction or Operculum Removal
For pericoronitis caused by an impacted wisdom tooth, the dentist may first try to irrigate and clean the area, then prescribe antibiotics. If the tooth continues to cause problems, extraction is the definitive solution.
In some cases, only the gum flap — the operculum — needs to be surgically removed if the tooth itself is properly positioned.
Home Remedies to Relieve Swollen Gum Around One Back Tooth
Home remedies provide temporary relief while you wait for your dental appointment. They do not treat the root cause — but they reduce pain and inflammation significantly.
Warm Saltwater Rinse
Dissolve half a teaspoon of salt in a glass of warm water. Swish gently for 30 seconds and spit. Repeat three to four times daily.
Saltwater helps reduce bacterial activity, soothe inflamed tissue, and promote early healing. It is safe, inexpensive, and recommended by dentists as a first-line home remedy.
Cold Compress on the Cheek
Apply a cold pack or ice wrapped in a cloth to the outside of your cheek near the swollen area. Hold it for 15 minutes on and 15 minutes off.
Cold reduces swelling and numbs localized pain without any medication. It is especially useful in the first 48 hours after swelling begins.
Antiseptic Mouthwash
Rinsing with an alcohol-free antiseptic mouthwash twice daily helps reduce bacterial load in the affected area. Look for chlorhexidine-based products or those with cetylpyridinium chloride.
Mouthwash cannot remove existing tartar, but it slows the growth of new bacteria and provides some anti-inflammatory benefit in the short term.
Gentle Flossing and Brushing
Carefully floss around the swollen tooth to remove any trapped food debris. Use a soft-bristled toothbrush and gentle circular motions around the gum line.
Avoid aggressive scrubbing which can damage already inflamed tissue. Clean gently but thoroughly. Often, removing the trapped irritant is enough to start visible improvement within 24 hours.
Over-the-Counter Pain Relievers
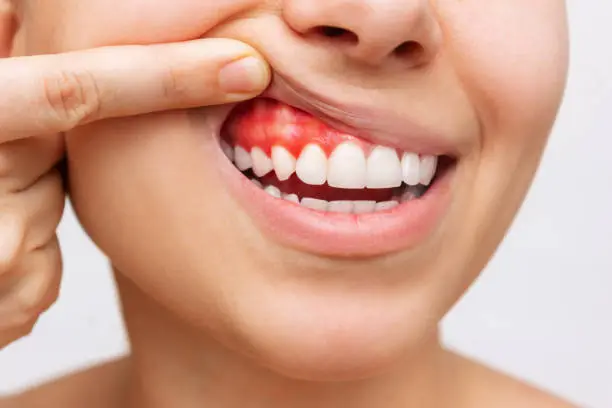
Ibuprofen is the most effective over-the-counter option because it both reduces pain and decreases inflammation. Take as directed on the label.
Acetaminophen reduces pain but not inflammation. It is a good alternative for people who cannot take ibuprofen. Neither medication should replace dental treatment.
Clove Oil Application
Clove oil contains eugenol, a natural anesthetic and antibacterial compound. Apply a tiny amount to a cotton ball and gently press it against the swollen gum for a few minutes.
This provides fast, temporary numbing relief. Do not apply it directly to open tissue or use too frequently, as it can irritate the gum if overused.
Oil Pulling With Coconut Oil
Swish one tablespoon of coconut oil in your mouth for 10 to 15 minutes, then spit it into the trash. Coconut oil contains lauric acid, which has antimicrobial properties.
Research suggests oil pulling can reduce bacterial counts in the mouth. It works best as a supplemental hygiene practice alongside brushing, flossing, and professional care.
Home Remedies vs. Professional Treatments — A Comparison
| Treatment Type | Best For | Duration of Relief | Fixes Root Cause |
|---|---|---|---|
| Saltwater rinse | Mild irritation, post-procedure care | Hours | No |
| Cold compress | Pain and swelling reduction | Hours | No |
| Ibuprofen | Pain and inflammation | 4–6 hours | No |
| Clove oil | Numbing pain temporarily | 1–2 hours | No |
| Professional cleaning | Gingivitis and plaque buildup | Long-term | Yes |
| Scaling and root planing | Periodontitis | Long-term | Yes |
| Root canal | Pulp infection, abscess | Permanent | Yes |
| Tooth extraction | Severe damage, impacted wisdom tooth | Permanent | Yes |
| Antibiotics | Infection control | Short-term support | Partial |
When to See a Dentist Immediately
Some situations require urgent dental care. Do not wait for a scheduled appointment if you experience any of these warning signs.
Swelling that spreads from the gum into your cheek, jaw, or neck needs same-day emergency care. A spreading infection can block your airway if it progresses unchecked.
Pus draining from the gum is a clear sign of abscess. Fever combined with gum swelling signals that the infection has entered your bloodstream. Difficulty swallowing or opening your mouth fully points to a serious deep-tissue infection.
Swelling that has lasted longer than one week without improvement needs professional evaluation even if pain is mild. Persistent low-grade swelling often indicates advancing gum disease or a developing infection that will worsen over time.
How to Prevent Swollen Gum Around One Back Tooth
Prevention is straightforward and consistent. Most localized gum swelling around back teeth is caused by inadequate cleaning and delayed dental visits.
Brush twice daily using a soft-bristled toothbrush and fluoride toothpaste. Angle the bristles at 45 degrees toward the gumline and use gentle circular strokes. Spend extra time on the back molars where plaque accumulates fastest.
Floss every single day to remove food particles and plaque from between teeth and below the gumline. A water flosser can help reach deep between back teeth. If traditional floss is difficult, interdental brushes are an effective alternative.
Use an antibacterial mouthwash daily to reduce bacterial load along the gumline. Products containing chlorhexidine or essential oils provide additional protection beyond brushing and flossing.
Visit your dentist every six months for professional cleaning and examination. A hygienist can remove tartar buildup that no toothbrush can reach. Your dentist can spot early signs of gum disease, decay, and cracks before they become serious problems.
Eat a balanced diet rich in vitamin C, calcium, and phosphorus. Vitamin C is essential for gum tissue integrity and immune defense. Calcium and phosphorus strengthen tooth enamel and the bone supporting your teeth.
Avoid tobacco in all forms. Smoking and chewing tobacco significantly increase your risk of gum disease, slow healing, and impair your immune response to gum infections.
Wear a nightguard if you grind your teeth during sleep. Bruxism creates microscopic cracks in back teeth and puts excessive pressure on the gum tissue, making it more susceptible to swelling and infection.
Swollen Gum Around One Tooth in the Back — Risk Factors
Some factors increase your likelihood of developing localized gum swelling behind a back tooth.
| Risk Factor | How It Contributes |
|---|---|
| Poor oral hygiene | Plaque and tartar buildup irritates gums |
| Age over 30 | Risk of periodontal disease increases significantly |
| Smoking or tobacco use | Weakens immune response, increases bacterial load |
| Diabetes | Impairs healing and increases infection risk |
| Dry mouth (Xerostomia) | Reduces saliva’s natural antibacterial protection |
| Vitamin C deficiency | Weakens gum tissue integrity and healing |
| Pregnancy | Hormonal changes increase gum sensitivity |
| Bruxism (teeth grinding) | Damages teeth and stresses gum tissue |
| Misaligned teeth | Creates hard-to-clean areas where bacteria collect |
| Previous gum disease history | Increases risk of recurrence and progression |
Swollen Gum Behind Back Tooth With No Wisdom Teeth
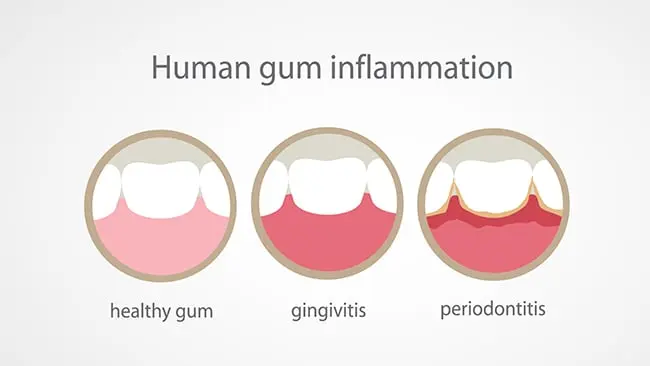
Many people experience swollen gum at the very back of their mouth but have already had their wisdom teeth removed. This is still very common and does not always relate to wisdom teeth.
The most frequent causes in this situation are food getting trapped in the extraction site if it healed poorly, gum disease targeting the last molar, a cracked second molar, or an abscess forming at the root tip of the back molar.
If you have had your wisdom teeth out but still experience swelling at the very back of your mouth, see your dentist. The cause is always something other than the wisdom tooth itself — and it needs to be identified.
Swollen Gum That Comes and Goes Around One Back Tooth
Intermittent swelling that appears and disappears around one back tooth is not something to dismiss. Recurring swelling almost always indicates an ongoing underlying problem.
Common causes of recurring localized swelling include a slow-draining abscess, a tooth with an incomplete root canal, advanced periodontitis with an active pocket, or a cracked tooth that continues to allow bacteria entry.
Each time the swelling goes down on its own, it may feel like the problem resolved. But if the underlying cause remains — bacteria, infection, or structural damage — the swelling will return, often worse each time.
Connection Between Gum Swelling and Overall Health
Research increasingly links periodontal disease to systemic health conditions. Chronic gum infection and inflammation do not stay confined to your mouth.
Studies have associated untreated periodontitis with increased risk of heart disease, stroke, diabetes complications, premature birth, and respiratory infections. The bacteria responsible for gum disease can enter the bloodstream through inflamed gum tissue and travel to other organs.
This is one more reason why swollen gum around one tooth in the back should never be ignored. Treating it is not just about your smile — it is about your whole body’s health.
Frequently Asked Questions (FAQs)
Why is my gum swollen around one tooth in the back but there is no pain?
Painless gum swelling is still a sign of infection or gum disease and needs dental evaluation. Gum disease often progresses painlessly until it becomes severe.
Can trapped food cause a swollen gum around one back tooth?
Yes, food debris stuck under the gumline is one of the most common causes. Careful flossing and rinsing often resolve it within one to two days.
How long does it take for a swollen gum around one tooth to go away?
Minor irritation-related swelling clears up within two to seven days with good hygiene. Swelling from infection or gum disease requires professional treatment to resolve fully.
Is a swollen gum around one back tooth a dental emergency?
It becomes an emergency if you have pus, fever, difficulty swallowing, facial swelling, or spreading pain. These require same-day dental care without delay.
Can I use a saltwater rinse to treat swollen gum around one back tooth?
Yes, warm saltwater rinses reduce bacterial activity and soothe inflamed tissue. They provide temporary relief but do not cure the underlying cause of the swelling.
What is pericoronitis and why does it cause swelling at the back of the mouth?
Pericoronitis is inflammation of the gum around a partially erupted wisdom tooth. Food and bacteria trap under the gum flap, causing significant pain and swelling at the very back of the mouth.
Can gum swelling around one tooth lead to tooth loss?
Yes. If the cause — particularly periodontitis or abscess — is left untreated, it can destroy the bone and tissue supporting the tooth, resulting in tooth loss over time.
Should I take antibiotics for a swollen gum around one back tooth?
Antibiotics are only appropriate when prescribed by a dentist for confirmed infection. They control the spread of bacteria but do not replace the dental treatment needed to fix the root cause.
Can I brush a swollen gum around a back tooth?
Yes, but gently. Use a soft-bristled toothbrush and light pressure. Avoiding the area entirely allows more plaque and bacteria to accumulate, which worsens the swelling.
When should I go to the ER for a swollen gum around one back tooth?
Go to the emergency room immediately if you have severe facial swelling, difficulty breathing or swallowing, high fever, or swelling spreading rapidly into your neck. These are signs of a serious, life-threatening infection.
Conclusion
Why is my gum swollen around one tooth in the back has many answers — and all of them require your attention.
Whether the cause is trapped food, early gingivitis, a dental abscess, an impacted wisdom tooth, or a cracked molar, the swelling is your body’s clear signal that something is wrong in that specific area.
The good news is that most causes are highly treatable when caught early. Home remedies like saltwater rinses and cold compresses provide short-term relief, but professional dental treatment is essential to eliminate the root cause and prevent the problem from returning.
In 2026, dental care is more accessible and advanced than ever before. Do not ignore localized gum swelling, do not wait until the pain becomes unbearable, and do not assume it will go away on its own.
Schedule a dental appointment, get the right diagnosis, and protect both your oral health and your overall well-being for the long term.
