Why are my gums receding is a question millions of people ask every year — and for good reason. Receding gums are one of the most common dental problems, yet most people do not notice them until real damage has already occurred.
The gum tissue slowly pulls away from the teeth, exposing sensitive roots and creating the perfect environment for bacteria to thrive. Left untreated, it can lead to tooth loss.
What Are Receding Gums?
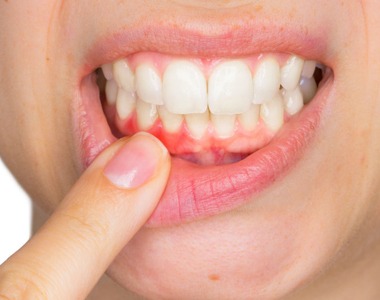
Receding gums, also called gum recession or gingival recession, happen when the gum tissue surrounding your teeth wears away or pulls back.
This exposes more of the tooth — and sometimes the tooth root itself. It creates small gaps or pockets between the teeth and gums where bacteria can collect and cause further damage.
The condition affects more than two-thirds of the population worldwide. The California Dental Association estimates that three out of every four adults have some form of periodontal disease, which includes gum recession.
Why Are My Gums Receding? The 10 Main Causes
Understanding what causes your gums to recede is the first step toward stopping it. There is rarely just one cause — most cases involve a combination of factors.
1. Periodontal Disease (Gum Disease)
Periodontal disease is the number one cause of receding gums. It is a bacterial infection that destroys the gum tissue and supporting bone that hold your teeth in place.
It begins as gingivitis — mild inflammation of the gums — and progresses into periodontitis if left untreated. At that stage, pockets form between the teeth and gums, and tissue destruction becomes severe.
Studies show that most adults over 30 have some degree of periodontal disease, and the risk increases with age.
2. Aggressive or Incorrect Brushing
Brushing too hard or using the wrong technique is one of the most common — and most avoidable — causes of gum recession.
Using a hard-bristled toothbrush and scrubbing aggressively wears away both enamel and gum tissue over time. Research has confirmed that hard bristles directly contribute to gingival recession.
It often occurs in people over 40 who have otherwise maintained good oral hygiene — the damage is simply the result of years of overly vigorous brushing.
3. Poor Oral Hygiene
Insufficient brushing, skipping flossing, and not rinsing with antibacterial mouthwash allows plaque to accumulate along and below the gum line.
Plaque that is not removed hardens into tartar (calculus) — a substance that can only be removed by a dental professional. Tartar buildup triggers inflammation and gum recession.
4. Genetics
Some people are simply more predisposed to gum disease and recession due to genetics. Studies show that up to 30% of the population may be genetically susceptible — regardless of how diligently they care for their teeth.
Inherited traits like naturally thin gum tissue, the position of teeth, and gum tissue composition can all increase the risk.
5. Tobacco Use
Smoking and chewing tobacco are directly linked to receding gums. Tobacco reduces blood circulation in the mouth, limiting the nutrients and oxygen gum tissue needs to stay healthy.
Tobacco users are also more likely to develop sticky plaque that is difficult to remove. This combination makes tobacco use one of the most damaging habits for gum health.
6. Bruxism (Teeth Grinding and Clenching)
Grinding or clenching your teeth — often during sleep — places excessive mechanical force on the teeth and gums. This constant pressure weakens the supporting gum tissue and causes it to pull away from the teeth over time.
Many people grind their teeth without knowing it. Signs include worn-down teeth, jaw pain, and morning headaches.
7. Hormonal Changes
Fluctuations in female hormones during puberty, pregnancy, and menopause can make gum tissue more sensitive and more vulnerable to recession.
These hormonal changes alter how gums respond to plaque and bacteria, increasing the risk of inflammation and tissue damage even with normal hygiene habits.
8. Misaligned Teeth or Abnormal Bite
When teeth do not come together properly, too much force is placed on certain areas of the gum tissue and bone. This imbalanced pressure can push the gums back over time.
Misaligned or crooked teeth also make it harder to clean the gum line properly, allowing plaque to build up in hard-to-reach areas.
9. Lip and Tongue Piercings
Jewelry worn in the lip or tongue can continuously rub against the gum tissue. This constant friction irritates and gradually wears away the gums, particularly on the lower front teeth.
10. Orthodontic Treatment
When teeth are moved orthodontically into areas with thin or insufficient bone, gum recession can occur as the bone in those areas is lost during tooth movement. Careful orthodontic planning is essential to minimize this risk.
Complete Causes at a Glance
| Cause | Risk Level | Controllable? |
|---|---|---|
| Periodontal disease | Very High | Yes (with treatment) |
| Aggressive brushing | High | Yes |
| Poor oral hygiene | High | Yes |
| Genetics | Moderate–High | No |
| Tobacco use | High | Yes |
| Teeth grinding (bruxism) | Moderate | Yes (with night guard) |
| Hormonal changes | Moderate | Partially |
| Misaligned teeth | Moderate | Yes (orthodontics) |
| Lip/tongue piercings | Moderate | Yes |
| Orthodontic movement | Low–Moderate | Partially |
Warning Signs: How Do I Know My Gums Are Receding?
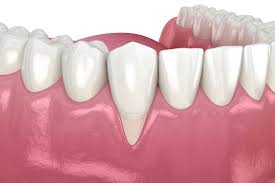
Gum recession develops gradually and is often painless in the early stages. Many people do not realize it is happening until significant tissue is already lost.
These are the warning signs to watch for:
Teeth That Look Longer Than Usual
If your teeth appear longer when you look in the mirror, your gums are likely pulling back. The tooth is not growing — the gum tissue covering it is receding.
This is one of the most noticeable visual signs and often the first one people spot in photos.
Tooth Sensitivity to Hot, Cold, or Sweet
Sensitivity is often one of the earliest indicators of gum recession. As the gum recedes, the tooth root becomes exposed.
Unlike the crown of the tooth, which is protected by hard enamel, the root is covered only by cementum — a much softer material. When exposed, temperature and sweetness easily reach the nerve, causing sharp, sudden sensitivity.
A Notch at the Gum Line
Running your tongue along the base of your teeth, you may feel a visible notch or groove where the crown meets the root. This physical boundary is a clear sign of recession.
Bleeding Gums
Gums that bleed when you brush or floss — especially consistently — signal active inflammation. Inflammation weakens gum tissue and causes it to pull away from the tooth surface.
Bleeding gums are often an early sign of gingivitis, which, if untreated, can progress to full gum recession.
Visible Root Exposure
In more advanced cases, you may actually be able to see the darker, yellower surface of the tooth root below what was previously the gum line.
Root surfaces are more porous and susceptible to decay than enamel, so root exposure significantly raises the risk of cavities at the gum line.
Loose or Shifting Teeth
When gum tissue recedes significantly, the bone and connective tissue that anchor the teeth can also be lost. This causes teeth to feel loose or to shift position.
Loose teeth are a serious sign that the supporting structures are compromised and immediate dental attention is needed.
Persistent Bad Breath
Bacteria that accumulate in the pockets created by receding gums can cause chronic bad breath. If brushing does not resolve persistent bad breath, it may be a sign that bacteria are building up beneath the gum line.
Pain or Discomfort at the Gum Line
Tenderness, pressure, or aching along the gum line — especially when chewing — can indicate that gum tissue is inflamed and receding.
Warning Signs Summary Table
| Warning Sign | What It Indicates | Urgency |
|---|---|---|
| Teeth look longer | Visible gum pulling back | Moderate — see dentist soon |
| Tooth sensitivity | Exposed root surfaces | Moderate |
| Notch at gum line | Physical recession boundary | Moderate |
| Bleeding gums | Active inflammation/gingivitis | Moderate — seek evaluation |
| Visible root exposure | Advanced recession | High — act quickly |
| Loose teeth | Bone and tissue loss | Very High — urgent care needed |
| Persistent bad breath | Bacterial pocket activity | Moderate |
| Gum line pain | Tissue inflammation | Moderate–High |
Stages of Gum Recession
Gum recession does not happen overnight. It progresses through distinct stages, each with its own symptoms and treatment needs.
Stage 1: Mild Recession
This is the earliest stage. The gum tissue begins to pull back slightly, exposing a small amount of the tooth root.
Symptoms may be subtle — slight sensitivity, gums that appear marginally lower. Many people overlook this stage entirely.
This is the best time to intervene. Improved oral hygiene habits and a dentist visit can often stop progression at this point.
Stage 2: Moderate Recession
The gums have receded further, and a noticeable portion of the tooth root is exposed. Sensitivity becomes more persistent, particularly with hot, cold, or sweet foods.
Teeth start to visibly look longer. Deeper pockets form between the gum and tooth, creating ideal conditions for bacterial buildup.
Treatment at this stage typically involves scaling and root planing (deep cleaning) and may include antibiotic therapy.
Stage 3: Advanced Recession
The most severe stage. Significant gum tissue is lost, teeth may appear dramatically longer, and loose teeth or tooth loss becomes a real risk.
Severe sensitivity, pain, and visible gaps between teeth are common. Surgical intervention — including gum grafting — is usually required at this stage.
Stage 4: Severe / End-Stage Recession
At this point, the supporting bone and connective tissue have been severely compromised. Teeth may fall out or require extraction.
Reconstructive procedures including bone grafting and gum grafting are needed, often followed by dental implants or other restorative options.
Can Receding Gums Grow Back?

This is one of the most common questions — and the answer is no.
Once gum tissue is lost, it does not regenerate on its own the way skin does. Gum recession is not reversible without professional treatment.
However, the good news is that treatment can stop further recession, restore lost tissue through surgical procedures, and significantly improve both function and appearance.
This is why catching it early is so important. Mild recession caught in Stage 1 may only require habit changes. Advanced recession in Stage 3 or 4 requires surgery.
Treatment Options for Receding Gums
The right treatment depends on the stage of recession and its underlying cause.
Non-Surgical Treatments
Scaling and Root Planing (Deep Cleaning)
This is the first-line non-surgical treatment for gum recession caused by periodontal disease.
The dentist or hygienist removes plaque and tartar from below the gum line, then smooths the root surfaces to make it harder for bacteria to reattach. This helps the gum tissue reattach to the tooth.
Desensitizing Agents and Fluoride Varnish
For patients experiencing pain or sensitivity, dentists can apply fluoride varnish or desensitizing agents to the exposed root surfaces.
At home, desensitizing toothpastes containing ingredients like potassium nitrate, stannous fluoride, or arginine can help calm nerve sensitivity over several weeks of use.
Antibiotics and Antimicrobial Rinses
Antibiotics may be prescribed — in gel, oral, or mouthwash form — to eliminate infection in the periodontal pockets. They are often used alongside deep cleaning to improve results.
Composite Restoration
A dentist can use tooth-colored composite resin to cover the exposed root surface and fill gaps between teeth caused by recession. This improves both sensitivity and aesthetics.
Surgical Treatments
Open Flap Scaling and Root Planing (Flap Surgery)
Used when non-surgical deep cleaning has not been sufficient. The periodontist folds back the gum tissue, removes bacteria and tartar from deeper below the surface, then secures the gum snugly back around the tooth.
This reduces pocket depth and eliminates more bacteria than standard cleaning.
Connective Tissue Graft (Soft Tissue Graft)
The most commonly performed gum surgery for recession. A small flap is made in the roof of the mouth (palate), and tissue from beneath it is taken and stitched to the area of recession.
This covers the exposed root and restores the gum line. It is highly effective and well-studied.
Free Gingival Graft
Instead of taking tissue from beneath a flap, tissue is taken directly from the surface of the palate. This is often used for patients who need to thicken thin gum tissue rather than just extend coverage.
Pedicle Graft
If enough healthy gum tissue surrounds the affected tooth, a flap of tissue from nearby can be stretched over the recession rather than taking tissue from the palate. Less invasive but not always possible.
Pinhole Surgical Technique
A minimally invasive alternative to traditional grafting. The periodontist makes a tiny hole in the gum tissue and uses special instruments to loosen and reposition it over the recession.
No cutting or suturing is required. Recovery is faster, though not all patients are suitable candidates.
Bone Regeneration
If bone loss has occurred alongside gum recession, regenerative procedures using membranes, bone graft materials, or tissue-stimulating proteins can encourage the body to rebuild lost bone.
This is combined with gum surgery when both tissue and bone need restoration.
Orthodontic Treatment
In cases where recession is driven by misaligned teeth or bite issues, orthodontic treatment slowly repositions the teeth. This redistributes pressure more evenly and can improve the gum margin over time.
Treatment Comparison Table
| Treatment | Type | Best For | Invasiveness |
|---|---|---|---|
| Scaling and root planing | Non-surgical | Early/moderate recession | Low |
| Desensitizing agents | Non-surgical | Sensitivity management | Minimal |
| Antibiotics | Non-surgical | Infection control | Minimal |
| Composite restoration | Non-surgical | Root coverage, aesthetics | Low |
| Flap surgery | Surgical | Moderate recession with deep pockets | Moderate |
| Connective tissue graft | Surgical | Moderate to severe recession | Moderate–High |
| Free gingival graft | Surgical | Thin gum tissue | Moderate |
| Pedicle graft | Surgical | Localized recession | Moderate |
| Pinhole technique | Minimally invasive | Moderate recession | Low |
| Bone regeneration | Surgical | Bone and tissue loss | High |
How to Prevent Receding Gums
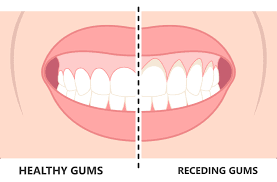
Prevention is always better than treatment. Many cases of gum recession are entirely preventable with the right habits.
Brush the Right Way
Use a soft-bristled toothbrush and brush in gentle, circular motions. Never scrub back and forth across the gum line.
Brush for two minutes, twice a day. Replace your toothbrush every three months, or sooner if the bristles are frayed.
Floss Every Day
Flossing removes plaque from between the teeth and along the gum line — areas your toothbrush simply cannot reach.
Skipping flossing means bacteria and plaque remain in these spaces, increasing the risk of gingivitis and recession.
See Your Dentist Every Six Months
Regular professional cleanings remove tartar that brushing and flossing cannot. Your dentist can also spot early signs of recession long before you notice them yourself.
Even with perfect home hygiene, professional cleanings are essential because tartar buildup above and below the gum line can only be removed with professional tools.
Quit Smoking and Tobacco
If you smoke or use any tobacco products, stopping is one of the most impactful things you can do for your gum health.
Tobacco restricts blood flow, impairs healing, and dramatically increases the risk of gum disease and recession.
Wear a Night Guard for Bruxism
If you grind or clench your teeth — even unconsciously during sleep — a custom-fitted night guard can protect your teeth and gums from the mechanical damage of bruxism.
Talk to your dentist if you wake up with jaw soreness or notice worn-down teeth.
Use Antimicrobial Mouthwash
Adding an antimicrobial mouthwash to your daily routine helps reduce bacteria in areas that brushing and flossing miss.
Look for products that specifically target gingivitis and plaque bacteria.
Eat a Gum-Healthy Diet
Nutrients matter for gum health. Vitamin C in particular is essential for gum tissue integrity. Foods rich in vitamin C — like citrus fruits, bell peppers, and broccoli — help keep gum tissue strong.
Limit sugar and acidic foods and drinks, which fuel bacterial growth and enamel erosion.
Address Bite Issues Early
If your dentist notes misaligned teeth or an uneven bite, addressing it with orthodontic treatment protects the gum tissue from uneven pressure over the long term.
The Link Between Receding Gums and Overall Health
Gum health does not exist in isolation. Research consistently links periodontal disease — the leading cause of gum recession — to systemic health conditions.
Studies correlate periodontal disease with an increased risk of heart disease, stroke, and type 2 diabetes. The underlying connection appears to be inflammation — when gum tissues are chronically inflamed, the inflammatory response can affect blood vessels and other tissues throughout the body.
This is not just a dental issue. Protecting your gums protects your overall health.
When to See a Dentist About Receding Gums
You should not wait for a scheduled check-up if you notice any of the following:
Persistent tooth sensitivity that does not improve. Gums that appear lower on any tooth than they used to. Bleeding gums during brushing or flossing that does not resolve within two weeks. Any visible root exposure. Loose or shifting teeth. Chronic bad breath that brushing does not fix.
The earlier gum recession is diagnosed and treated, the simpler and less invasive the treatment will be. Ignoring it allows the condition to progress to stages that require surgery.
Frequently Asked Questions (FAQs)
Why are my gums receding even though I brush regularly?
Brushing too hard can cause gum recession even with good hygiene. Genetics, hormonal changes, and underlying periodontal disease can also cause recession regardless of brushing habits.
Can receding gums grow back on their own?
No. Once gum tissue is lost it does not regenerate naturally. Professional treatments like gum grafting can restore tissue, but the gums will not grow back without intervention.
What does a receding gum line look like?
The teeth appear longer than normal, a visible notch or line may appear at the gum line, and the root surface — which is darker and yellower than the crown — may be visible.
Is gum recession painful?
Early gum recession is often painless. The most common symptom is tooth sensitivity to hot, cold, or sweet — sharp discomfort that signals the root is exposed.
How is gum recession diagnosed?
A dentist uses a small probe to measure the depth of gum pockets around each tooth. Healthy pockets measure 1–3 mm. Anything over 5 mm indicates significant periodontal disease and recession.
What is the best treatment for receding gums?
For mild recession, scaling and root planing (deep cleaning) is typically the first step. For moderate to severe cases, soft tissue graft surgery or the pinhole technique is the most effective option.
Does gum recession affect only older people?
No. While it is more common in adults over 40, gum recession can affect people of any age, especially those with aggressive brushing habits, genetic predisposition, or early-onset gum disease.
Can bruxism (teeth grinding) cause gum recession?
Yes. The excessive mechanical force from grinding and clenching puts stress on the gum tissue and supporting bone, causing the gums to pull back over time.
How can I stop my gums from receding further?
Switch to a soft-bristled toothbrush, brush gently, floss daily, quit tobacco, use an antimicrobial mouthwash, wear a night guard if you grind, and see your dentist every six months for professional cleaning.
Is gum recession related to serious health conditions?
Yes. Research links chronic periodontal disease — the leading cause of gum recession — to increased risk of heart disease, stroke, and type 2 diabetes due to the body-wide effects of chronic inflammation.
Conclusion
Why are my gums receding is not a question to sit on. Gum recession is a progressive condition that starts silently and worsens without intervention.
From aggressive brushing and gum disease to genetics and hormonal changes, the causes are varied — but the consequences are consistent.
Left untreated, receding gums lead to sensitivity, root decay, bone loss, and eventually tooth loss. The encouraging truth is that modern dentistry offers a full range of effective treatments, from non-invasive deep cleaning to advanced gum grafting procedures, that can stop recession in its tracks and restore your gum line.
The key is acting early. If your teeth look longer than before, feel more sensitive, or your gums bleed regularly, do not wait.
Schedule an appointment with your dentist today and take the first step toward protecting your smile and your long-term health.
