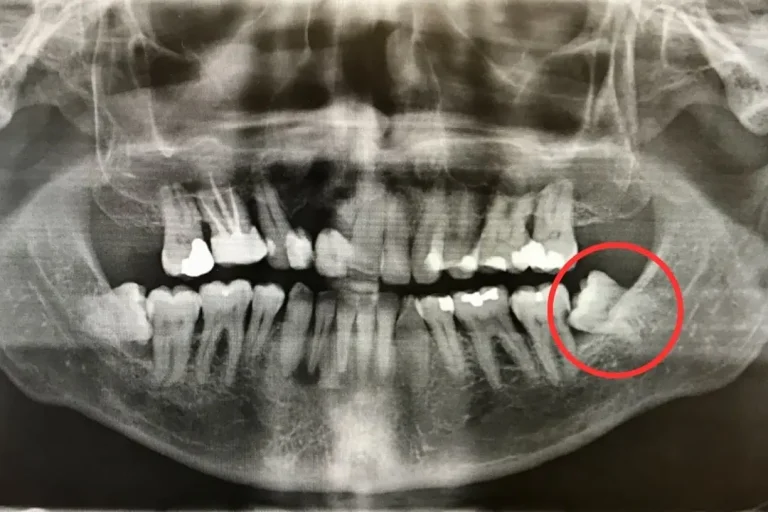
Why experts now say not to remove your wisdom teeth is a question reshaping modern dentistry across the world.
For decades, pulling third molars was considered routine, almost a rite of passage for teenagers and young adults.
But the science has shifted. Leading dental researchers and oral health organizations now question whether most of these extractions were ever necessary.
If your dentist has recommended wisdom tooth removal and you’re not in pain.
What Are Wisdom Teeth and Why Do We Have Them?
Wisdom teeth are your third set of molars, located at the very back of your mouth. They typically emerge between ages 17 and 25, which is why they’re called “wisdom” teeth — they arrive at a more mature age.
Our ancient ancestors had larger jaws and rougher diets. These extra molars helped grind tough, unprocessed foods like roots, nuts, and raw meat.
As human diets evolved and jaw sizes shrank over generations, wisdom teeth became less necessary. Today, they often don’t have enough room to grow in properly — but that doesn’t automatically mean they need to be removed.
The Old Thinking: Remove Them Before They Cause Problems
For most of the 20th century, dentists followed a simple philosophy — extract wisdom teeth early as a preventive measure.
The logic was that these teeth would eventually cause crowding, infections, or impaction. Better to remove them before problems developed, the thinking went.
This approach turned wisdom tooth extraction into one of the most common surgical procedures in the world. In the United States alone, around 5 million people have their wisdom teeth removed each year, costing over $3 billion annually.
Why the Science Has Changed
Recent research has fundamentally challenged the “remove them just in case” approach.
Studies now show that up to 60% of wisdom tooth removals may be unnecessary. A significant portion of wisdom teeth never cause any harm at all — they simply sit quietly at the back of the mouth without disrupting anything.
The current consensus among evidence-based dental researchers is clear: there are no scientifically proven health benefits to removing wisdom teeth that are not causing problems.
What the Research Actually Shows
| Finding | Detail |
|---|---|
| Unnecessary removals | Up to 60% of extractions may not be medically needed |
| Problem-free impacted teeth | About 30% of impacted wisdom teeth never cause issues |
| Correctly aligned wisdom teeth | Around 35% of people develop wisdom teeth that grow in properly |
| People with no wisdom teeth | Around 35% of people never develop wisdom teeth at all |
| Annual US extractions | Approximately 5 million people, costing over $3 billion |
These numbers make it clear that routine removal is not the evidence-based choice it was once believed to be.
The Real Risks of Wisdom Tooth Extraction
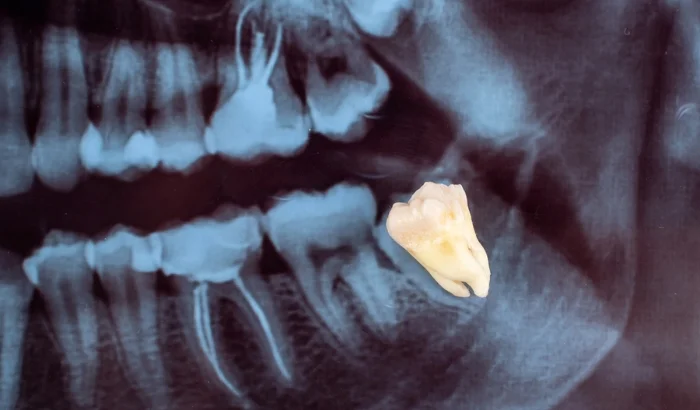
Wisdom tooth removal is not a minor procedure. It is oral surgery, and like all surgery, it carries real risks.
Dental professionals who now advocate for a more conservative approach point to these complications as a key reason to avoid unnecessary extraction.
Dry Socket (Alveolar Osteitis)
Dry socket is one of the most common post-extraction complications. It occurs when the blood clot that forms in the empty socket is dislodged or dissolves too early, exposing raw bone and nerve tissue.
The result is intense, radiating pain that can last for days. It often has a foul odor or taste and requires additional dental visits for treatment.
Dry socket occurs in about 4% of all extractions, but the risk rises significantly for lower wisdom teeth, smokers, women on oral contraceptives, and patients over 30. In high-risk groups, rates can approach 30% or more.
Nerve Damage
The lower wisdom teeth sit close to the inferior alveolar nerve and the lingual nerve. Both can be damaged during extraction.
Nerve injury can cause numbness, tingling, or altered sensation in the lips, tongue, chin, and cheeks. Most nerve numbness is temporary, resolving within 4–8 weeks. But permanent nerve damage, while rare, does occur in approximately 1–5% of cases.
For a procedure performed on a healthy tooth that wasn’t causing any symptoms, that risk becomes very difficult to justify.
Other Surgical Complications
| Complication | Approximate Rate |
|---|---|
| Dry socket | 3–10% (higher for lower molars) |
| Postoperative infection | About 1.7% |
| Temporary nerve numbness | 5–8% of mandibular extractions |
| Permanent nerve damage | 0.04–1.5% |
| Sinus perforation (upper teeth) | Rare but possible |
| Jaw fracture | Very rare |
Every one of these risks becomes unnecessary when the wisdom teeth being removed were healthy and problem-free to begin with.
What “Minimally Invasive Dentistry” Means and Why It Matters
The shift away from routine wisdom tooth removal is part of a larger movement called minimally invasive dentistry.
This philosophy holds that the best dental treatment is the least treatment necessary. Preserving natural tooth structure — including wisdom teeth — is prioritized over prophylactic removal.
Modern diagnostic tools like digital X-rays, cone beam CT scans, and 3D imaging allow dentists to assess wisdom tooth position, root structure, and proximity to nerves with incredible precision.
Instead of guessing what might happen in the future, dentists can now monitor wisdom teeth accurately over time and intervene only if a genuine problem develops.
Benefits of Keeping Your Wisdom Teeth
If your wisdom teeth are healthy, properly positioned, and not causing symptoms, there are real advantages to keeping them.
Extra Chewing Surface
Properly aligned wisdom teeth function as full molars. They add additional surface area for grinding and chewing food, contributing to efficient digestion.
Jaw Structure Support
Natural teeth help maintain the density and structure of your jawbone. Removing teeth, including wisdom teeth, can lead to bone loss in that area over time.
Backup Molars
If you lose one of your other molars due to injury or disease later in life, a healthy wisdom tooth can step in as a functional replacement.
No Surgical Risk or Recovery
Keeping healthy wisdom teeth means avoiding anesthesia, post-operative pain, dietary restrictions, and recovery time altogether. That’s not a small benefit.
Financial Savings
Wisdom tooth extraction, especially complex surgical removal, is expensive. The procedure can cost anywhere from $300 to over $1,000 per tooth, not including anesthesia, follow-up visits, or treatment of complications.
When Wisdom Tooth Removal IS Still Necessary
Experts who advocate against routine removal are not saying wisdom teeth should never come out. There are clear situations where extraction is the right call.
You Need Removal If
- Your wisdom teeth are impacted (stuck beneath the gum line or bone) and causing pain or infection
- You have pericoronitis — a recurring infection of the gum tissue around a partially erupted wisdom tooth
- The tooth is causing decay in itself or the adjacent second molar
- Wisdom teeth are creating overcrowding that is visibly shifting other teeth
- A cyst or tumor has formed around an impacted tooth
- The position of the tooth makes it structurally impossible to clean
- Your dentist has documented progression — a tooth that was monitored and is now causing measurable damage
The key word throughout all of this is “causing.” The decision should be based on what the teeth are actually doing, not what they might hypothetically do someday.
Quick Reference: Keep vs. Remove
| Situation | Recommendation |
|---|---|
| Fully erupted, properly aligned, no symptoms | Monitor and keep |
| Partially erupted but clean, no infection | Monitor closely |
| Impacted with no pain, no damage to neighbors | Active surveillance |
| Causing repeated infections (pericoronitis) | Remove |
| Decayed tooth or damaging adjacent molar | Remove |
| Cyst or tumor formation | Remove immediately |
| Overcrowding causing bite shift | Evaluate and likely remove |
The Role of Individual Dental Anatomy
One of the most important shifts in modern dental thinking is the move away from one-size-fits-all treatment.
Every patient’s jaw size, tooth position, bone density, and oral hygiene habits are different. A wisdom tooth that would be problematic in one person’s mouth might be perfectly stable in another’s.
Factors that influence whether wisdom teeth can safely stay include:
- Jaw size and whether there is adequate room for the teeth
- The angle at which the teeth are growing (vertical, horizontal, or angled)
- How much of the crown is exposed versus covered by gum tissue
- The distance between wisdom tooth roots and the inferior alveolar nerve
- Your ability to clean the back of your mouth effectively
- Your overall oral hygiene and gum health history
A thorough evaluation by a trusted dental professional — including X-rays and a clinical exam — should form the basis of any decision.
How to Properly Monitor Your Wisdom Teeth
If you and your dentist decide to keep your wisdom teeth under surveillance, here is what that monitoring process should look like.
Regular Dental Checkups
Visit your dentist every 6 to 12 months. At each appointment, your dentist should visually inspect the wisdom teeth and surrounding gum tissue for signs of redness, swelling, or pocketing.
Periodic X-Rays
Dental X-rays, typically every 1–2 years, help track changes in tooth position and identify issues that aren’t yet visible or painful, such as early decay or root contact with adjacent teeth.
Watch for Warning Signs
Between dental visits, pay attention to any of the following:
- Persistent pain or pressure at the back of the jaw
- Swollen, red, or bleeding gums around the wisdom teeth
- Difficulty opening your mouth fully
- Bad breath or a bad taste that doesn’t go away with brushing
- Pain radiating to the ear or jaw
Any of these symptoms should prompt an immediate dental appointment, not a wait-and-see approach.
Oral Hygiene Tips for Keeping Your Wisdom Teeth Healthy
Wisdom teeth are harder to clean than other teeth because of their position at the back of the mouth. Good hygiene habits are non-negotiable if you plan to keep them.
Brushing
Use a soft-bristled toothbrush and angle it carefully toward the gumline at the back of your mouth. An angled or compact head toothbrush makes it easier to reach the last molar.
Electric toothbrushes with small rotating heads are particularly effective for cleaning wisdom teeth.
Flossing
Standard floss can be difficult to maneuver around wisdom teeth. Try floss picks, interdental brushes, or a water flosser to clean between the wisdom tooth and the second molar.
Antiseptic Mouthwash
A daily antibacterial rinse like chlorhexidine or fluoride mouthwash can help reduce bacterial buildup around wisdom teeth that are partially erupted.
Dietary Awareness
Crunchy, sticky, or very sugary foods get trapped around wisdom teeth more easily. Rinsing after meals and maintaining a balanced diet reduces the risk of decay.
What to Do If Your Dentist Recommends Extraction
If you’re not in pain and your dentist recommends removing your wisdom teeth, here is a practical approach to handling that conversation.
Ask why, specifically. Ask your dentist to explain exactly what they see on your X-rays and clinical exam that justifies removal. A good dentist will walk you through the findings.
Ask about active surveillance. Request the option of monitoring rather than immediate extraction if no acute problem exists right now.
Get a second opinion. You have every right to consult a different dentist or an oral surgeon before agreeing to surgery. A second opinion on elective dental surgery is entirely reasonable.
Research their reasoning. Understand the difference between “this tooth may cause a problem” and “this tooth is causing a problem.” Only the latter is a clear indication for surgery.
Consider the cost-benefit ratio. Weigh the financial cost and medical risk of surgery against the actual, documented risk that your specific wisdom teeth pose to your oral health.
The Broader Shift in Dental Philosophy
The wisdom teeth debate reflects something bigger happening in healthcare generally — a move toward evidence-based medicine and away from procedures rooted in habit rather than proof.
For decades, the default was to remove wisdom teeth because “that’s what we’ve always done.” The burden of proof was on keeping them, not on removing them.
That has reversed. The current evidence-based position places the burden of proof on justifying extraction. If there is no clear clinical indication, the default should be to monitor and preserve.
This shift protects patients from unnecessary surgical risk, unnecessary cost, and unnecessary loss of natural tooth structure.
Summary: Key Takeaways at a Glance
| Topic | Key Point |
|---|---|
| Historical approach | Routine preventive removal for all patients |
| Current expert consensus | Remove only when clinically indicated |
| Unnecessary extraction rate | Up to 60% of removals may not be needed |
| Main risks of extraction | Dry socket, nerve damage, infection, sinus issues |
| Benefits of keeping wisdom teeth | Chewing function, jaw support, backup molars, no surgery risk |
| When to remove | Impaction with symptoms, infection, decay, cysts, crowding |
| Best monitoring strategy | Biannual checkups plus periodic X-rays |
| Your rights | Always ask for reasons, get a second opinion if unsure |
Frequently Asked Questions (FAQs)
Why do experts now say not to remove wisdom teeth?
Current research shows that up to 60% of wisdom tooth extractions may be unnecessary. Healthy, asymptomatic wisdom teeth carry no proven need for removal, while the surgery itself carries real risks.
Are wisdom teeth useful for anything?
Yes. Properly aligned wisdom teeth provide extra chewing surface, help maintain jaw bone density, and can serve as backup molars if other teeth are lost later in life.
What happens if I keep my impacted wisdom teeth?
Many impacted wisdom teeth never cause problems at all. Studies show about 30% of impacted teeth remain problem-free. Regular monitoring through X-rays and checkups is typically sufficient.
What are the biggest risks of wisdom tooth removal?
The main risks include dry socket (affecting 3–10% of extractions), nerve damage causing temporary or permanent numbness, postoperative infection, and in rare cases sinus perforation or jaw fracture.
How do I know if my wisdom teeth actually need to come out?
Clear signs include persistent pain, recurring gum infections (pericoronitis), tooth decay involving the wisdom tooth or adjacent molar, visible crowding, or cyst formation. Discomfort alone is not always a sufficient reason.
Can wisdom teeth cause crowding if I leave them in?
The evidence on wisdom teeth causing front tooth crowding is weak. Most dental researchers now agree that lower teeth tend to crowd with age regardless of whether wisdom teeth are present.
Is it safe to monitor wisdom teeth instead of removing them?
Yes. Active surveillance with regular dental checkups and X-rays every 6–12 months is a well-accepted, evidence-based approach recommended by major dental health organizations.
How do I clean wisdom teeth properly to avoid problems?
Use an angled toothbrush, interdental brushes or a water flosser to clean between the wisdom tooth and the molar in front of it. Antibacterial mouthwash also helps reduce bacterial buildup.
Should I get a second opinion before wisdom tooth removal?
Absolutely. If your dentist recommends extraction and you are not experiencing acute pain or infection, seeking a second opinion from another dentist or oral surgeon is a reasonable and smart step.
At what age is it too late to remove wisdom teeth?
There is no hard age limit, but extraction is generally easier in younger patients when roots are not fully formed. That said, healthy wisdom teeth at any age are better left in place unless problems arise.
Conclusion
Why experts now say not to remove your wisdom teeth comes down to one fundamental principle — unnecessary surgery is bad medicine.
The evidence is clear that millions of wisdom tooth extractions have been performed on healthy teeth that posed no real threat to oral health.
Every one of those procedures carried risk of dry socket, nerve damage, infection, and prolonged recovery, all for a tooth that was not causing any harm.
The modern approach is smarter, more personalized, and more patient-centered. If your wisdom teeth are healthy, properly positioned, and manageable with good oral hygiene, there is no clinical basis for removing them.
Regular monitoring, diligent home care, and an open conversation with a dentist you trust are all you need.
If your wisdom teeth are causing documented, measurable problems — pain, infection, decay, crowding — then extraction is absolutely the right decision.
But that choice should be based on what is actually happening in your mouth, not on outdated assumptions about what might happen someday.
Protect your natural teeth, ask the hard questions, and always make sure the recommendation to operate is backed by real evidence.