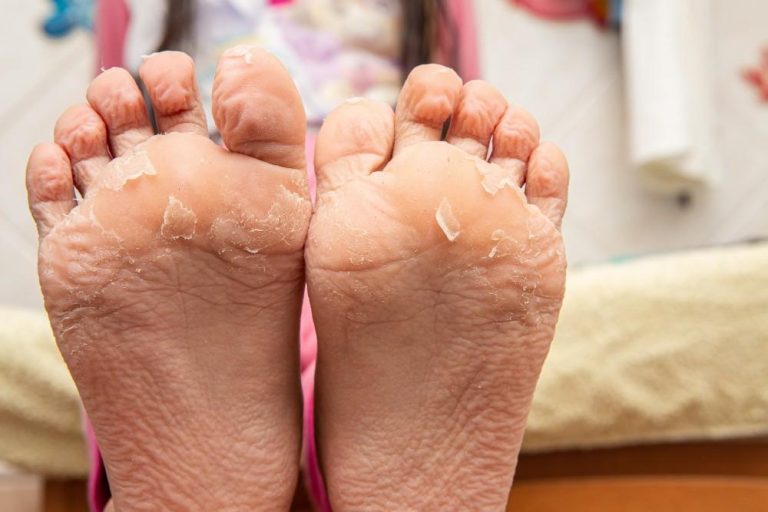
Why are my feet peeling is one of the most searched foot health questions in 2026, and for good reason.
Peeling skin on the feet is incredibly common and can range from a minor annoyance to a sign of something that needs medical attention.
Whether you are noticing flaky skin between your toes, peeling on the bottom of your feet, or shedding skin on your heels, this guide covers every cause, every fix, and every warning sign you need to know.
What Does It Mean When Your Feet Are Peeling?
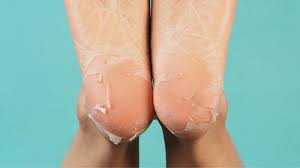
Peeling feet simply means the outer layer of your skin is shedding faster than it should. Your skin naturally renews itself every few weeks, but when something disrupts that process, you get visible peeling.
The shedding can look like thin flakes, large sheets of skin, or rough dry patches. Some people experience peeling between the toes, others on the soles or heels.
Most causes of why your feet are peeling are treatable at home. However, some cases signal an underlying condition that requires professional care.
Why Are My Feet Peeling? 12 Common Causes
1. Dry Skin (Xerosis)
Dry skin is the single most common reason why feet peel. The skin on your feet has fewer oil glands than the rest of your body, making it naturally prone to moisture loss.
Heat, low humidity, long hot showers, dehydration, stress, and aging all strip moisture from the skin barrier. When the skin gets too dry, it cracks, flakes, and peels.
This is especially noticeable on the heels, balls of the feet, and outer edges of the big toes. Cold weather and central heating make it significantly worse.
2. Athlete’s Foot (Tinea Pedis)
Athlete’s foot is one of the top causes of peeling feet. It is a contagious fungal infection that thrives in warm, moist environments like sweaty shoes, locker rooms, public showers, and pool decks.
The fungus (dermatophytes) attacks the outer skin layer and causes itchy, scaly, peeling skin, often starting between the toes and spreading to the soles and sides of the feet.
About 70% of people will experience athlete’s foot at some point in their lives. It is highly contagious and can be picked up from contaminated floors, shared towels, or borrowed shoes.
Key symptoms:
- Itching and burning between toes
- Scaly, flaking skin on soles
- Redness and inflammation
- Unpleasant foot odor
- Blisters that may burst and peel
3. Eczema (Atopic Dermatitis)
Eczema is an inflammatory skin condition that can cause dry, itchy, cracked, and peeling skin on the feet. It is more common in people who also have asthma or allergies.
Dyshidrotic eczema specifically affects the hands and feet. It causes tiny fluid-filled blisters on the toes and soles that itch intensely before peeling or breaking open.
Eczema flares up in response to heat, stress, allergens, and certain soaps or detergents. It is not contagious but can be persistent without proper management.
4. Psoriasis
Psoriasis is a chronic autoimmune condition that speeds up skin cell turnover. Skin cells build up faster than they can shed, forming thick, scaly patches that peel away.
Palmoplantar psoriasis specifically affects the palms and soles of the feet. You may notice red, raised, flaking patches that look silvery or gray and may be itchy or painful.
Unlike dry skin, psoriasis does not respond to moisturizer alone. It requires targeted medical treatment, often including topical steroids or prescription creams.
5. Contact Dermatitis
Contact dermatitis happens when the skin reacts to an irritant or allergen it has come into direct contact with. On the feet, this is often caused by shoe materials.
Rubber, dyes, adhesives, leather-tanning chemicals, and synthetic sock fabrics are all common triggers. The rash often matches the shape of the shoe strap or toe box where contact occurred.
Symptoms include redness, itching, dryness, and peeling. People who wear steel-toed boots or non-breathable footwear are especially prone to this type of reaction.
6. Hyperhidrosis (Excessive Sweating)
Hyperhidrosis is a condition where you sweat excessively, even without physical activity or heat. When feet stay constantly damp, the skin barrier breaks down.
Waterlogged skin becomes soft, white, and prone to maceration, a process where skin becomes overly saturated and begins to peel, especially between the toes.
Hyperhidrosis also creates the perfect warm, moist environment for fungal and bacterial infections, which further accelerate peeling.
7. Sunburn
Many people forget to apply sunscreen to their feet when wearing sandals or going barefoot. Sunburned skin on the feet follows the same pattern as anywhere else on the body.
A day or two after the burn, the damaged outer skin layer begins to peel as the body sheds dead cells. This is especially common on the tops of the feet and toes.
Walking barefoot on hot sand or concrete can also cause a mild burn that leads to peeling days later.
8. Allergic Reactions
Some people develop an allergic reaction to materials found in footwear or nail products. This is a form of allergic contact dermatitis.
Common allergens include rubber compounds, metal hardware, certain dyes, and formaldehyde resins used in shoe manufacturing. Even some medicated foot creams can trigger reactions in sensitive people.
The peeling is often localized to the area that was in direct contact with the allergen.
9. Keratolysis Exfoliativa
Keratolysis exfoliativa is a harmless condition that causes superficial peeling of the skin on the palms and soles. It is more common in warm weather or after water exposure.
It appears as air-filled blisters that rupture and leave behind peeling, flaking skin. There is usually no itching, pain, or redness, which distinguishes it from athlete’s foot.
The exact cause is not fully understood, but it tends to improve on its own. Gentle moisturizing can speed up recovery.
10. Diabetes
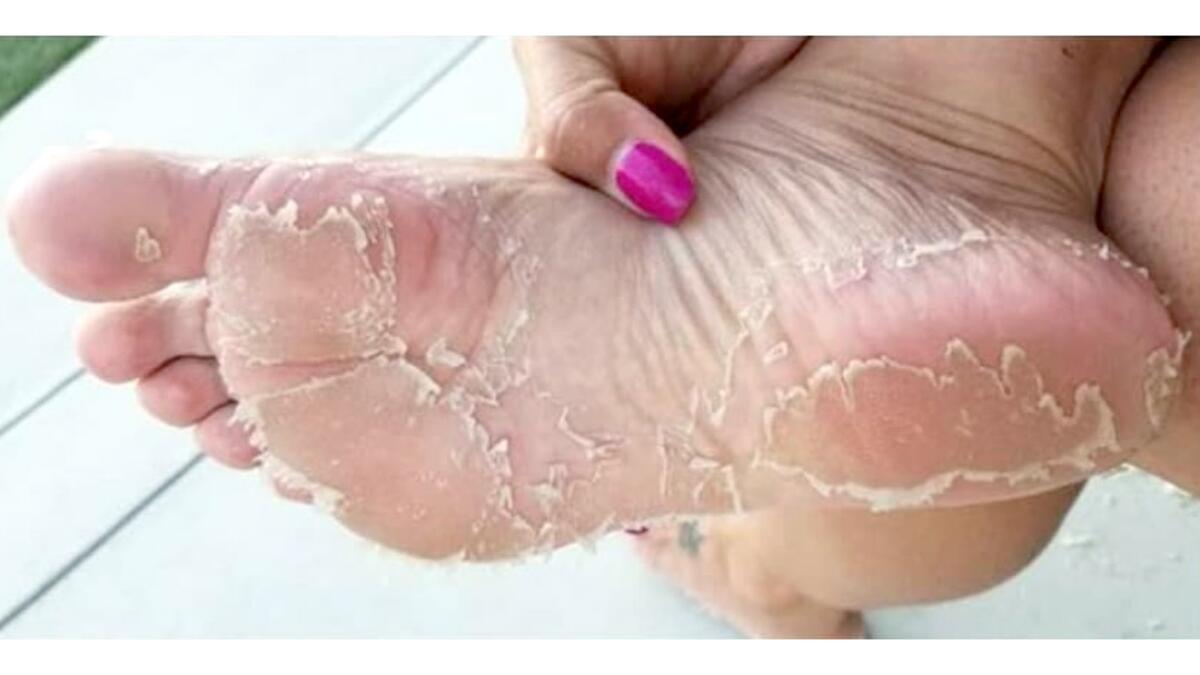
Diabetes can affect the blood supply to the feet, leading to poor circulation and nerve damage. This combination causes skin to become very dry and prone to cracking and peeling.
Diabetic skin heals more slowly, which means peeling skin can quickly become a serious concern. Even minor cuts, sores, or cracks can develop into complications if not treated promptly.
Anyone with diabetes who notices persistent peeling on their feet should consult both a dermatologist and a podiatrist.
11. Hypothyroidism
An underactive thyroid gland produces insufficient thyroid hormone, which can cause widespread dry skin throughout the body, including the feet.
When thyroid levels are low, the skin loses its ability to retain moisture effectively. This leads to dry, rough, flaking, and peeling skin, particularly on the soles and heels.
If peeling feet are accompanied by fatigue, weight gain, cold sensitivity, or hair loss, a thyroid check may be warranted.
12. Aging
As we age, collagen production decreases and the skin’s ability to retain moisture diminishes. Older adults often notice significantly drier, more fragile skin on their feet.
The skin on aging feet becomes thinner, loses its natural oils faster, and is slower to heal. Peeling and cracking, particularly around the heels, become increasingly common.
Regular moisturizing becomes even more important with age to compensate for the reduced natural hydration.
Causes by Location: Where Your Feet Are Peeling Matters
| Location of Peeling | Most Likely Causes |
|---|---|
| Between the toes | Athlete’s foot, hyperhidrosis, contact dermatitis |
| Bottom of feet (soles) | Dry skin, psoriasis, eczema, keratolysis exfoliativa |
| Heels | Dry skin, xerosis, aging, diabetes |
| Tops of feet | Sunburn, contact dermatitis, eczema |
| Around toes/toenails | Fungal infection, psoriasis, eczema |
| Large sheets peeling | Athlete’s foot, sunburn, keratolysis exfoliativa |
| Small flakes | Dry skin, mild eczema, aging |
Symptoms to Watch For
Understanding your symptoms helps identify which cause is behind the peeling.
Itching + burning + odor between toes — most likely athlete’s foot (fungal infection)
Thick, scaly, silver-gray patches — likely psoriasis
Tiny blisters that peel — may be dyshidrotic eczema or keratolysis exfoliativa
Redness matching shoe shape — contact dermatitis or allergic reaction
Peeling after sun exposure — sunburn
White, soft, saturated skin — hyperhidrosis or prolonged moisture exposure
Dry, cracked heels with no itching — xerosis (dry skin), aging, or diabetes-related dryness
Easy Fixes: How to Treat Peeling Feet at Home
Moisturize Daily and Correctly
Daily moisturizing is the foundation of treatment for almost every cause of peeling feet. Apply a thick, fragrance-free cream or ointment right after bathing while skin is still slightly damp.
Avoid thin lotions on the feet. Look for products containing urea, lactic acid, salicylic acid, glycerin, or hyaluronic acid as these actively repair and hydrate the skin barrier.
Apply generously to soles and heels but avoid putting heavy ointments between the toes, as trapped moisture there can encourage fungal growth.
Use an OTC Antifungal for Athlete’s Foot
If itching, burning, and peeling between the toes point to athlete’s foot, start with an over-the-counter antifungal cream, spray, or powder. Common options include clotrimazole, terbinafine, and tolnaftate.
Apply as directed and continue for the full recommended duration even after symptoms clear. Stopping early leads to recurrence.
Keep feet dry, change socks frequently, and avoid walking barefoot in communal areas while treating the infection.
Exfoliate Gently
Removing dead skin helps treatments penetrate better and prevents buildup. Use a pumice stone or foot file after soaking feet in warm water for 10 to 15 minutes.
Gently rub rough areas on the heels and soles. Do not over-exfoliate or scrub raw or cracked areas.
Follow up immediately with moisturizer to lock in hydration after exfoliation.
Try the Overnight Moisturizing Method
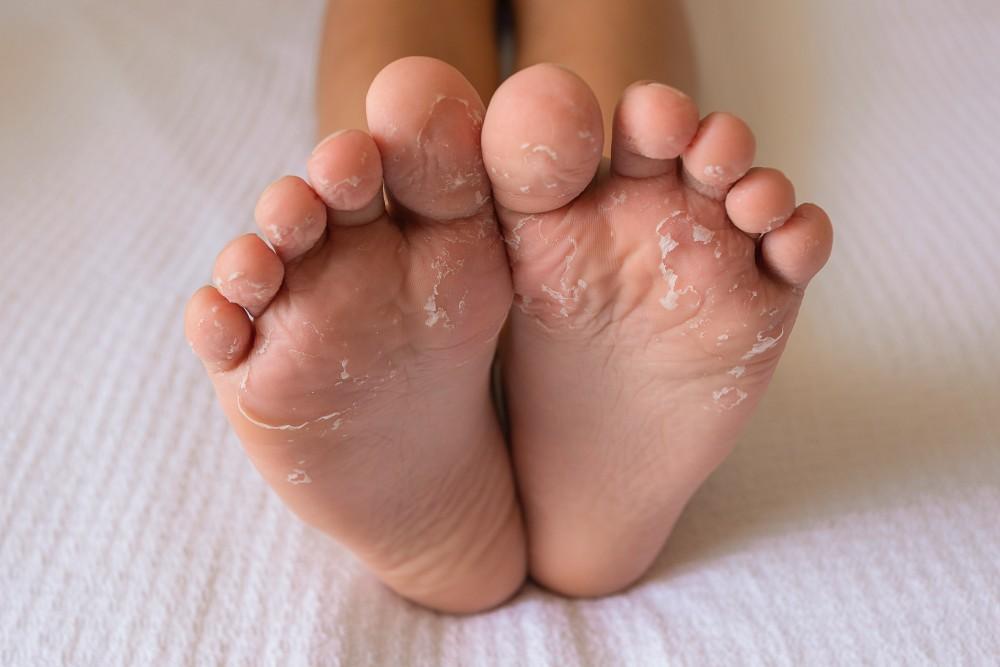
Apply a thick layer of urea-based cream or petroleum jelly to clean feet before bed. Put on a pair of cotton socks to lock in the moisture overnight.
This method is extremely effective for severely dry, cracked, or peeling heels. Consistent use for a week can produce dramatic improvement.
Cotton socks help the skin absorb the treatment without the heat buildup that synthetic materials can cause.
Soak Feet Regularly
A 15-minute warm water foot soak helps soften hardened, peeling skin. Adding a small amount of colloidal oatmeal, Epsom salts, or apple cider vinegar can soothe irritation.
Do not use very hot water, which strips natural oils and worsens dry skin. Warm water is always better.
After soaking, gently pat feet dry and apply moisturizer immediately before the skin has a chance to dry out completely.
Switch Socks and Footwear
Change to moisture-wicking or 100% cotton socks, especially if sweating is contributing to the problem. Change socks when damp, particularly after exercise.
Choose breathable footwear made from natural materials like leather or canvas. Avoid plastic-lined or non-ventilated shoes that trap heat and moisture.
Rotating between two or more pairs of shoes gives each pair time to dry out completely between wears.
Protect from Sunburn
Apply SPF 30 or higher sunscreen to the tops and sides of your feet whenever you wear sandals or go barefoot outdoors. Re-apply every two hours.
If a sunburn has already occurred, cool the skin with a cold compress, apply aloe vera gel, and stay out of the sun while healing.
Do not peel the sunburned skin manually. Let it shed naturally to avoid exposing raw skin underneath.
Address Contact Dermatitis
Identify and remove the offending material. Switch to unlined, breathable shoes made without rubber or synthetic dyes if those are suspected triggers.
Use fragrance-free and dye-free cleansers and moisturizers. Apply OTC hydrocortisone 1% cream for short-term itch and redness relief.
If symptoms persist after removing the trigger, consult a dermatologist for patch testing to identify the specific allergen.
Best Ingredients to Look For in Foot Creams
| Ingredient | What It Does | Best For |
|---|---|---|
| Urea (10–25%) | Breaks down dead skin, deep hydration | Dry skin, cracked heels, calluses |
| Lactic acid | Gentle exfoliation, moisture retention | Rough, thickened skin |
| Salicylic acid | Removes dead skin cells | Calluses, psoriasis, thickened patches |
| Glycerin | Draws moisture into skin | All types of dry, peeling skin |
| Hyaluronic acid | Deep hydration | Mild dryness, aging skin |
| Petroleum jelly | Seals in moisture | Cracked heels, overnight treatment |
| Shea butter | Softens and repairs barrier | Dryness, eczema, contact dermatitis |
| Tea tree oil | Natural antifungal properties | Mild athlete’s foot, fungal issues |
Prevention: How to Stop Feet From Peeling
Preventing peeling feet is far easier than treating them once they start. A few consistent habits make a significant difference.
Moisturize every day. Make it part of your post-shower routine. Applying cream to slightly damp skin after bathing is the most effective time.
Wear breathable footwear. Natural materials reduce heat and moisture buildup that trigger both dry skin and fungal infections.
Change socks when damp. This single habit dramatically reduces the risk of athlete’s foot and hyperhidrosis-related peeling.
Stay hydrated. Drinking enough water supports skin health from the inside out. Dehydration contributes to dryness across the whole body.
Wear footwear in communal areas. Flip-flops or shower shoes in gym changing rooms, public pools, and shared showers protect against fungal infection.
Avoid very hot showers. Hot water strips natural oils from the skin. Lukewarm water is much gentler and less drying.
Apply sunscreen to feet. Include the tops and sides of your feet in your sun protection routine whenever wearing sandals.
Trim toenails carefully. Improper nail trimming can create pressure points that damage surrounding skin and contribute to peeling.
Peeling Feet Prevention Checklist
| Habit | Frequency | Benefit |
|---|---|---|
| Moisturize after bathing | Daily | Prevents dry skin, heals cracks |
| Change socks when damp | As needed | Reduces fungal risk |
| Exfoliate with pumice stone | 2–3x per week | Removes dead skin buildup |
| Wear breathable shoes | Always | Reduces heat and moisture |
| Wear footwear in public showers | Always | Prevents athlete’s foot |
| Apply sunscreen to feet | When outdoors | Prevents sunburn peeling |
| Foot soak in warm water | 2–3x per week | Softens skin, aids treatment |
| Drink 8 glasses of water daily | Daily | Supports skin hydration |
When to See a Doctor About Peeling Feet
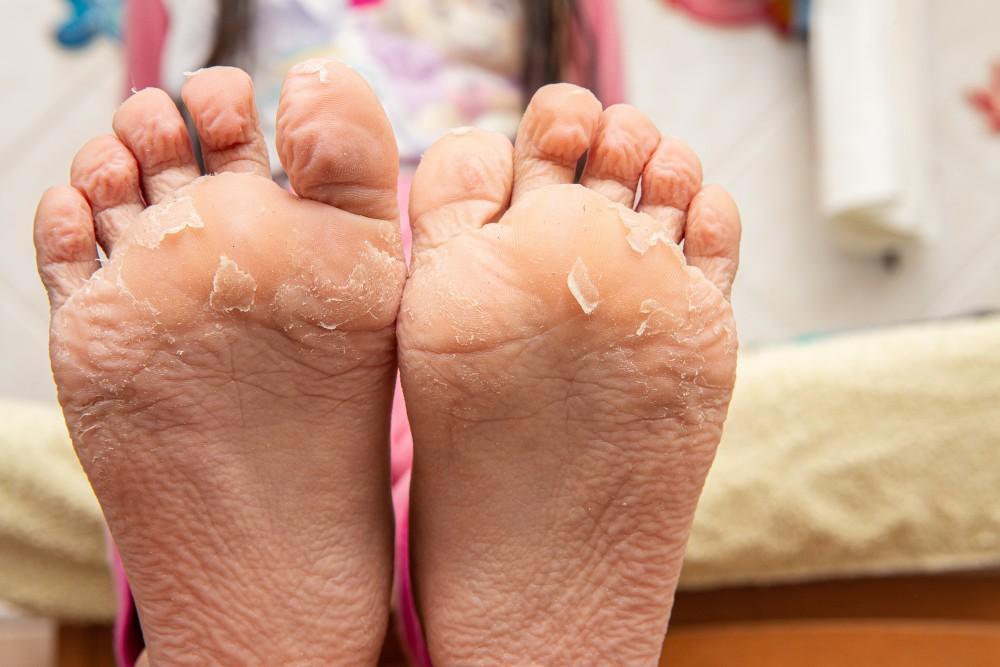
Most cases of why your feet are peeling clear up with home care. However, certain warning signs mean it is time to consult a podiatrist or dermatologist.
See a doctor if you notice:
- Peeling does not improve after two to four weeks of home treatment
- Skin is cracked, bleeding, or showing signs of infection
- Redness, swelling, warmth, or pus are present
- Peeling is accompanied by fever
- You have diabetes and any open skin on your feet
- Peeling returns repeatedly after treatment
- Deep heel fissures that limit your ability to walk comfortably
- Thick nail changes alongside skin peeling (possible nail fungus)
- Numbness or loss of sensation in the feet
Early professional care prevents small issues from becoming serious complications, especially for people with diabetes or circulation problems.
Medical Treatments for Persistent Peeling
When home remedies are not enough, doctors have a range of effective treatment options depending on the underlying cause.
For fungal infections: Prescription-strength topical antifungals or oral antifungal medications (terbinafine, fluconazole) for stubborn or widespread infections.
For eczema: Prescription topical steroids, tacrolimus ointment, or dupilumab injections for severe cases.
For psoriasis: Topical corticosteroids, vitamin D analogs, coal tar preparations, or biologics for severe presentations.
For hyperhidrosis: Prescription-strength aluminum chloride antiperspirant, glycopyrronium towelettes, Botox injections, or iontophoresis therapy.
For contact dermatitis: Patch testing to identify allergens, prescription anti-inflammatory creams, and guidance on footwear and material avoidance.
For diabetes-related peeling: Specialized wound care, diabetic footwear consultation, and a coordinated care plan with a podiatrist.
Peeling Feet in Children
Children can also experience peeling feet. The most common causes in kids include juvenile plantar dermatitis, athlete’s foot picked up from school gym floors or pools, dry skin from sandal-wearing, and mild eczema.
Make sure your child’s shoes fit correctly and are not creating friction hotspots. Always pair enclosed shoes with cotton socks.
Apply a child-safe, fragrance-free moisturizer to the feet regularly. If peeling is accompanied by itching, redness, or blisters, consult a pediatrician or podiatrist for diagnosis.
Seasonal Factors That Affect Foot Peeling
Certain seasons make peeling feet more likely. Knowing the seasonal triggers helps you adjust your foot care routine accordingly.
Summer: Sandal-wearing dries out unprotected skin. Increased sun exposure causes sunburn on tops of feet. Pool and locker room exposure raises fungal risk. Sweating in closed shoes promotes athlete’s foot.
Winter: Cold air combined with central heating dramatically drops humidity. Hot showers become more tempting but strip more moisture. Thick wool socks can cause friction. Reduced water intake leads to more dehydration.
Spring/Fall: Seasonal transitions cause skin to adjust to new temperatures and humidity levels. Contact dermatitis from new footwear purchased for the season is common.
Adjusting your moisturizing routine by season, particularly applying richer creams in winter and using antifungal powder in summer, keeps peeling under control year-round.
Peeling Feet vs. Normal Skin Shedding: What Is the Difference?
Your skin naturally replaces itself every 28 to 30 days. Some mild flaking is completely normal as dead cells shed.
The concern arises when peeling is excessive, affects large areas, comes with other symptoms like itching or burning, or does not respond to basic moisturizing.
If you are finding flakes of skin in your socks or on your floor regularly, or if the skin is coming off in visible sheets, that goes beyond normal cell turnover and deserves attention.
Frequently Asked Questions (FAQs)
Why are my feet peeling but not itchy?
Non-itchy peeling is most often caused by dry skin, sunburn, or keratolysis exfoliativa. These conditions do not typically trigger the immune response that causes itching, unlike fungal infections or eczema.
Can dehydration cause feet to peel?
Yes. When the body is dehydrated, the skin loses moisture faster than it can replenish it. This leads to dryness, cracking, and peeling, particularly on the soles and heels of the feet.
Why are the bottoms of my feet peeling?
The soles are under constant pressure and friction from walking. Combined with fewer oil glands, the bottoms of the feet are especially prone to dry skin, callus buildup, and conditions like psoriasis and athlete’s foot.
How do I stop my feet from peeling fast?
The fastest fix is daily moisturizing with a urea or lactic acid cream, the overnight sock method with petroleum jelly, and gentle exfoliation with a pumice stone two to three times per week. Eliminate hot showers and switch to breathable socks.
Is peeling skin between toes always athlete’s foot?
No, but athlete’s foot is the most common cause of inter-toe peeling. Other causes include hyperhidrosis (excess sweating), contact dermatitis, and maceration from moisture. Athlete’s foot is usually accompanied by itching and burning.
Can stress cause feet to peel?
Yes. Chronic stress raises cortisol levels, which disrupts the skin barrier and reduces its ability to retain moisture. Stress can also trigger eczema and psoriasis flare-ups, both of which cause peeling feet.
When should I see a doctor for peeling feet?
See a doctor if peeling persists beyond three to four weeks, is accompanied by bleeding, pus, or swelling, or you have diabetes and any open skin on your feet. Recurring peeling after treatment also warrants professional evaluation.
Does athlete’s foot cause peeling in large sheets?
Yes. Advanced athlete’s foot, particularly the moccasin-type variant, can cause the entire sole and sides of the foot to peel in large sheets. This type requires consistent antifungal treatment and may need prescription medication.
Can the wrong shoes cause feet to peel?
Absolutely. Ill-fitting shoes create friction and blisters that peel after they heal. Non-breathable materials trap heat and moisture, promoting fungal growth. Allergic materials in shoes can cause contact dermatitis with peeling.
Are peeling feet a sign of diabetes?
Peeling feet can be related to diabetes because poor circulation and nerve damage dry out the skin and slow healing. If you have diabetes and notice persistent peeling, cracking, or slow-healing skin on your feet, consult your podiatrist promptly.
Conclusion
Why are my feet peeling is a question with many answers, but most of them have straightforward solutions.
Whether the cause is something as simple as dry skin from not moisturizing regularly, a fungal infection picked up at the gym, or a chronic condition like eczema or psoriasis, understanding what is driving the peeling puts you in control of fixing it.
The key to healthy feet in 2026 is consistency. Moisturize daily, wear breathable footwear, change socks when damp, protect against sun exposure, and treat infections early before they spread. Most cases of peeling feet clear up within two to four weeks with the right care routine.
If your feet continue to peel despite home treatment, do not delay seeing a podiatrist or dermatologist. Some underlying causes like psoriasis, hyperhidrosis, or diabetes-related skin changes need professional attention to manage effectively.
Your feet carry you through every day, and they deserve the care and attention to stay healthy, smooth, and comfortable all year long.