Why am I not ovulating but having periods is one of the most common and confusing fertility questions women ask in 2026.
You get your period every month, so everything should be fine — right? Not always. It is entirely possible to have regular or irregular bleeding without actually releasing an egg.
This condition is called an anovulatory cycle, and it affects millions of women worldwide.
Understanding what is happening in your body, what causes it, and what you can do about it is the first step toward protecting your reproductive health and fertility goals.
What Does “Not Ovulating but Having Periods” Actually Mean?

When you ask why am I not ovulating but having periods, the answer lies in understanding the difference between true menstruation and anovulatory bleeding.
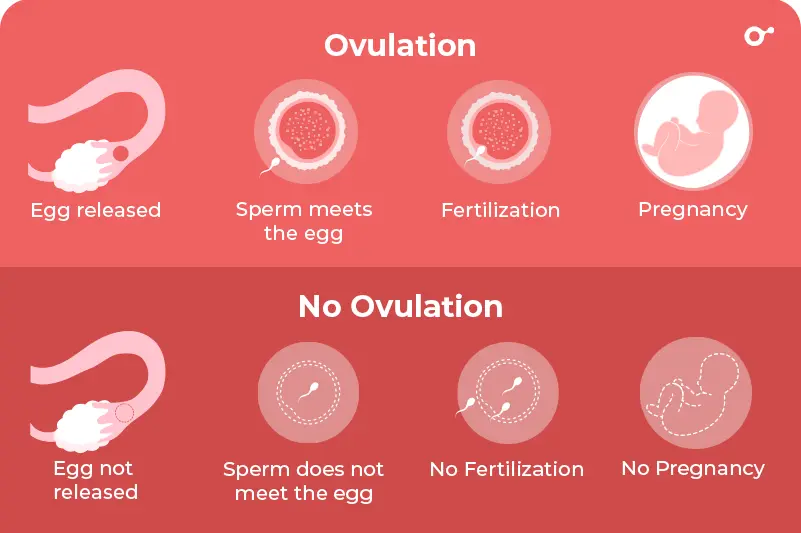
True menstruation only happens after ovulation. When an egg is released and not fertilized, progesterone drops and the uterine lining sheds — that is your period.
When you do not ovulate, the same bleeding event can still occur, but for a different reason. Estrogen builds up the uterine lining without progesterone to stabilize it. When estrogen eventually drops, the lining sheds — but this is called anovulatory bleeding, not a true period.
Around 30% of women experience at least one anovulatory cycle during their reproductive years without ever knowing it.
Understanding the Normal Ovulation Process
To understand why you are not ovulating but having periods, it helps to know how a healthy ovulatory cycle works.
The Follicular Phase Your brain releases follicle-stimulating hormone (FSH), which stimulates several follicles in the ovary to grow. Each follicle contains an immature egg. As they grow, they produce estrogen, thickening the uterine lining.
The LH Surge About 24 to 36 hours before ovulation, a surge in luteinizing hormone (LH) triggers the dominant follicle to rupture and release the mature egg. This is ovulation.
The Luteal Phase After the egg is released, the empty follicle becomes the corpus luteum. This structure produces progesterone, which maintains the uterine lining and supports a potential pregnancy.
Menstruation If fertilization does not occur, the corpus luteum breaks down, progesterone falls, and the uterine lining sheds as your period.
In an anovulatory cycle, the corpus luteum never forms. No progesterone is produced. The system is incomplete.
What Is Anovulation? A Clear Definition
Anovulation means your ovaries fail to release a mature egg during a menstrual cycle.
It is one of the leading causes of female infertility, responsible for approximately 30% of infertility cases in women according to the National Institutes of Health.
Anovulation can be chronic (happening consistently) or occasional (happening in isolated cycles). Both forms need attention if you are trying to conceive.
Anovulatory bleeding differs from a true period — it may be heavier, lighter, or arrive at irregular intervals. Many women cannot tell the difference without tracking fertility signs.
Top Causes of Not Ovulating but Having Periods
There are many reasons why a woman may experience bleeding without ovulation. Here are the most common causes.
Polycystic Ovary Syndrome (PCOS)
PCOS is the single most common cause of anovulation. It affects approximately 1 in 10 women of childbearing age in the United States.
PCOS causes the body to produce excess androgens (male hormones like testosterone). These high androgen levels prevent follicles from maturing and releasing eggs.
Women with PCOS often have irregular periods, acne, excess facial or body hair, and difficulty conceiving. Insulin resistance is also commonly present.
Thyroid Disorders
Both an underactive thyroid (hypothyroidism) and an overactive thyroid (hyperthyroidism) can disrupt ovulation.
Thyroid hormones directly influence the hormonal signals that trigger egg release. An imbalanced thyroid can interfere with FSH and LH levels, preventing ovulation.
Hypothyroidism also raises prolactin levels as a side effect, which further suppresses ovulation. Treating the thyroid often restores normal ovulation.
High Prolactin Levels (Hyperprolactinemia)
Prolactin is the hormone responsible for milk production. When prolactin is elevated outside of breastfeeding, it blocks the hormones needed for ovulation.
High prolactin can result from a small noncancerous pituitary tumor called a microadenoma, certain medications, stress, or thyroid dysfunction.
Once prolactin levels are brought back to normal range, ovulation typically resumes in 70 to 80% of women.
Low or High Body Weight (BMI Issues)
Body fat plays a direct role in hormone production. Both extremes — being underweight or overweight — can shut down ovulation.
A BMI under 18.5 can cause the pituitary gland to stop producing enough LH and FSH. Being overweight (BMI over 30) increases androgens and insulin resistance, disrupting the hormonal cycle.
Research shows that a BMI under 18.5 or over 30 raises the risk of anovulation by up to 300%.
Chronic Stress
Stress is one of the most overlooked causes of anovulation. When the body is under prolonged stress, it releases higher levels of cortisol.
Elevated cortisol suppresses GnRH (gonadotropin-releasing hormone), which is the master hormone that starts the ovulation cascade. Without GnRH, the entire cycle stalls.
Even moderate psychological stress sustained over weeks or months can delay or completely prevent ovulation in otherwise healthy women.
Excessive Exercise
High-intensity exercise for more than 60 minutes per day has been shown to increase anovulation risk significantly.
Extreme physical training depletes the body’s energy availability, causing the hypothalamus to scale back reproductive function as a protective response.
Female athletes and women training intensively for events often experience anovulatory cycles or even complete loss of their period (amenorrhea).
Perimenopause
As women approach their mid-40s, hormone production becomes increasingly erratic. The ovaries begin to respond less reliably to FSH signals.
Anovulatory cycles become much more common during perimenopause, even when bleeding continues. This is a natural hormonal transition, not a medical emergency.
However, anovulation during perimenopause still has implications for bone health, cardiovascular health, and cancer risk because of low progesterone levels.
Primary Ovarian Insufficiency (POI)
POI, sometimes called premature ovarian failure, occurs when the ovaries stop functioning normally before age 40.
Women with POI may still have occasional periods or bleeding, but ovulation occurs infrequently or not at all. The condition is associated with low estrogen and high FSH levels.
POI affects about 1 in 100 women under 40 and can be caused by genetics, autoimmune conditions, or previous medical treatments.
Hormonal Birth Control (Recent or Ongoing)
Coming off hormonal birth control can temporarily disrupt ovulation. The pill, patch, injection, and hormonal IUDs all work partly by suppressing ovulation.
After stopping hormonal contraception, some women experience a lag period of several months before the hypothalamic-pituitary-ovarian axis fully reactivates.
This is sometimes called post-pill anovulation and typically resolves within 3 to 6 months, though it can take longer in some cases.
Causes of Anovulation: Quick Reference Table
| Cause | Key Hormone Disrupted | How Common |
|---|---|---|
| PCOS | Androgens, LH, Insulin | 1 in 10 women |
| Thyroid Disorders | TSH, Prolactin | Very common |
| High Prolactin | Prolactin suppresses LH/FSH | Common |
| High/Low BMI | Androgens, FSH, LH | Very common |
| Chronic Stress | Cortisol suppresses GnRH | Common |
| Excessive Exercise | GnRH, FSH, LH | Common in athletes |
| Perimenopause | Estrogen, FSH | Natural transition |
| Primary Ovarian Insufficiency | FSH elevated, Estrogen low | 1 in 100 under 40 |
| Post-Birth Control | LH, FSH temporarily suppressed | Common after stopping |
Signs and Symptoms of Not Ovulating

If you are wondering why am I not ovulating but having periods, these symptoms can help you identify what is going on.
Irregular Periods A cycle that varies wildly in length — sometimes 21 days, sometimes 45 days — is a classic sign of anovulation. A healthy ovulatory cycle is typically 24 to 35 days.
Very Heavy or Very Light Bleeding Anovulatory bleeding often differs from normal menstrual flow. Without progesterone to properly prepare and shed the lining, the bleeding can be unpredictably heavy or unusually light.
No Change in Cervical Mucus Around ovulation, cervical mucus becomes clear, slippery, and stretchy — like raw egg whites. If you never notice this type of discharge mid-cycle, you may not be ovulating.
No Basal Body Temperature (BBT) Rise After ovulation, progesterone causes a small but measurable rise in resting body temperature (roughly 0.2°C or 0.4°F). A flat BBT chart with no spike after mid-cycle is a strong indicator of anovulation.
Negative Ovulation Predictor Kit (OPK) Results OPKs detect the LH surge that precedes ovulation. Consistently negative OPK results around mid-cycle suggest the LH surge is not occurring.
Infertility If you have been trying to conceive for 6 to 12 months without success while having regular cycles, anovulation may be the underlying cause.
Absence of Premenstrual Symptoms Breast tenderness, bloating, and mood changes before a period are largely driven by progesterone. If you never experience PMS-type symptoms, low progesterone (from lack of ovulation) may be the reason.
Symptoms Comparison: Ovulatory vs. Anovulatory Cycle
| Sign | Ovulatory Cycle | Anovulatory Cycle |
|---|---|---|
| Cervical Mucus | Clear, stretchy, egg-white mid-cycle | Absent or always thick/pasty |
| BBT Pattern | Rise of ~0.2°C after ovulation | Flat — no rise |
| OPK Result | Positive LH surge detected | Negative or no surge |
| Period Regularity | Consistent cycle length | Variable, irregular |
| Bleeding | Moderate, predictable | Heavy, light, or unpredictable |
| PMS Symptoms | Present (breast tenderness, bloating) | Absent or minimal |
| Progesterone Level | Rises in luteal phase | Stays low all cycle |
How to Confirm You Are Not Ovulating
There are several ways to find out whether you are ovulating — at home and with your doctor.
Track Your Basal Body Temperature Use a basal thermometer every morning before getting out of bed. Record results daily. Look for a sustained rise of about 0.2°C in the second half of your cycle. No rise means no ovulation.
Use Ovulation Predictor Kits (OPKs) OPKs test urine for the LH surge that triggers egg release. Test once daily from day 10 of your cycle onward. Consistently negative results in multiple cycles suggest anovulation.
Monitor Cervical Mucus Observe your vaginal discharge daily throughout the cycle. The absence of slippery, egg-white cervical mucus near mid-cycle is a reliable sign of anovulation.
Mid-Luteal Progesterone Blood Test A blood test 7 days after suspected ovulation (around day 21 in a 28-day cycle) measures progesterone levels. A level below 3 ng/mL typically confirms that ovulation did not occur.
Follicular Ultrasound Monitoring A doctor can use transvaginal ultrasound to watch follicle development throughout your cycle and confirm whether an egg is released. This is the most definitive diagnostic method.
Other Hormonal Blood Tests Doctors may also check FSH, LH, estradiol, prolactin, thyroid-stimulating hormone (TSH), testosterone, and anti-Müllerian hormone (AMH) to identify the underlying hormonal cause.
Diagnostic Tests for Anovulation
| Test | What It Measures | When It Is Done |
|---|---|---|
| Mid-Luteal Progesterone | Confirms ovulation occurred | Day 21 (or 7 days after suspected ovulation) |
| FSH and LH | Pituitary signals to ovaries | Cycle day 2–3 |
| AMH (Anti-Müllerian Hormone) | Ovarian reserve / egg count | Any day of cycle |
| Prolactin | Elevated = suppresses ovulation | Cycle day 2–3 |
| TSH (Thyroid) | Thyroid function | Any day |
| Estradiol | Estrogen baseline | Cycle day 2–3 |
| Testosterone / DHEA | Rule out PCOS / androgen excess | Any day |
| Transvaginal Ultrasound | Follicle development, ovary structure | Multiple days in cycle |
Medical Treatments for Anovulation
If lifestyle changes are not enough, several medical treatments are available to stimulate or restore ovulation.
Clomiphene Citrate (Clomid) Clomid is the most commonly prescribed first-line fertility medication for anovulation. It works by blocking estrogen receptors in the brain, tricking the body into producing more FSH.
Studies show that within six cycles of Clomid use, approximately 40 to 45% of women achieve pregnancy. It is relatively low-cost and noninvasive.
Letrozole (Femara) Letrozole is an aromatase inhibitor originally developed for breast cancer. It is now widely used off-label for ovulation induction, especially in women with PCOS who do not respond to Clomid.
Many reproductive endocrinologists now prefer letrozole over Clomid because it carries a lower risk of multiple pregnancies and produces a more natural hormonal profile.
Metformin For women with PCOS and insulin resistance, metformin (a diabetes medication) can help regulate insulin levels and indirectly restore ovulation.
Metformin is often used alongside letrozole or Clomid to improve response, particularly in women with elevated blood sugar or metabolic syndrome.
Gonadotropin Injections (FSH/LH) Injectable gonadotropins directly stimulate the ovaries to produce and mature multiple follicles. They are used when oral medications fail.
These medications require close monitoring via ultrasound and blood work due to the risk of ovarian hyperstimulation syndrome (OHSS) and multiple pregnancies.
Bromocriptine or Cabergoline Used specifically when high prolactin levels are the cause of anovulation. These medications lower prolactin, allowing the normal hormonal cycle to resume.
Studies show that once prolactin normalizes, ovulation returns in approximately 70 to 80% of women.
IUI (Intrauterine Insemination) IUI is often combined with ovulation induction medication. When the egg is about to be released, sperm is directly placed into the uterus to increase the chances of fertilization.
IVF (In Vitro Fertilization) For severe cases of anovulation that do not respond to other treatments, IVF may be the most effective path. Eggs are retrieved, fertilized in a lab, and transferred back to the uterus.
Natural Ways to Support and Restore Ovulation
Many women want to know what they can do naturally before turning to medication. Here are evidence-based approaches.
Reach and Maintain a Healthy BMI Weight has one of the strongest effects on ovulation. Even losing 5% of body weight in women with obesity-related anovulation has been shown to significantly improve insulin sensitivity and hormone balance.
For underweight women, a modest weight gain of just a few kilograms can restart ovulation in women whose cycles have stopped due to low body weight.
Reduce Intense Exercise If you are training more than 60 minutes at high intensity daily, scaling back can help. Replacing some high-intensity sessions with yoga, walking, or swimming supports hormone balance without depleting energy reserves.
Manage Stress Actively Practices like mindfulness meditation, yoga, breathwork, and adequate sleep directly reduce cortisol levels. Lower cortisol allows GnRH to be released normally, restarting the ovulation cascade.
Improve Your Diet A low-glycemic, high-fiber diet rich in omega-3 fatty acids, plant proteins, and micronutrients supports hormonal balance. Reducing ultra-processed foods, refined carbohydrates, and trans fats improves insulin sensitivity and reduces androgen excess.
Consider Targeted Supplements Several supplements have research support for improving ovulation, particularly in women with PCOS. Always consult your doctor before starting any supplement.
| Supplement | Benefit | Best For |
|---|---|---|
| Inositol (Myo + D-Chiro) | Improves insulin sensitivity and ovulation | PCOS |
| Magnesium | Supports hormonal regulation | General cycle health |
| N-Acetyl Cysteine (NAC) | Improves ovulatory response | PCOS |
| Vitamin D | Deficiency linked to anovulation | Women with low vitamin D |
| Omega-3 Fatty Acids | Reduces inflammation, supports FSH | General fertility |
| Berberine | Improves insulin resistance | PCOS alternative to metformin |
| CoQ10 | Supports egg quality | Women over 35 |
Address the Root Cause If your anovulation is caused by thyroid disease, high prolactin, or PCOS, treating the underlying condition is more effective than general lifestyle changes alone. Work with a healthcare provider to identify and treat the specific cause.
When Should You See a Doctor?
You do not have to wait until you are struggling to conceive to take action.
See your doctor if your cycle length varies by more than 7 days from month to month. Irregular cycles lasting fewer than 21 days or longer than 35 days consistently also warrant evaluation.
Seek care if you have been trying to conceive for 12 months without success (or 6 months if you are over 35).
Also see a doctor if you have very heavy or very light periods, pelvic pain, signs of PCOS (acne, excess hair growth, weight gain around the abdomen), or you have not been able to detect any ovulation signs in multiple cycles.
Early evaluation makes treatment easier and outcomes better.
Impact of Anovulation on Long-Term Health
Not ovulating is not just a fertility issue — it has broader health consequences.
Estrogen Dominance and Endometrial Hyperplasia Without progesterone to balance estrogen, the uterine lining can grow excessively. This condition, called endometrial hyperplasia, increases the risk of endometrial cancer if left untreated for years.
Bone Health Progesterone and estrogen both play roles in maintaining bone density. Chronic anovulation, especially with low estrogen, accelerates bone loss and increases the risk of osteoporosis.
Cardiovascular Health Low progesterone and hormonal imbalance associated with long-term anovulation have been linked to higher cardiovascular risk in some studies.
Mental Health The hormonal fluctuations of an anovulatory cycle — particularly the absence of the progesterone-driven luteal phase — can contribute to mood instability, anxiety, and depressive symptoms.
Fertility Outlook: Can You Get Pregnant If You Are Not Ovulating?

The straightforward answer is no — you cannot conceive naturally without ovulation. Ovulation is required for an egg to be available for fertilization.
However, the outlook is generally positive. Most causes of anovulation are treatable. With proper diagnosis and treatment, many women with anovulation go on to achieve pregnancy.
PCOS, the most common cause, responds well to lifestyle changes and ovulation induction medications. Studies show Clomid and letrozole together achieve pregnancy in a large proportion of PCOS patients within 6 cycles.
Even in more complex cases like POI or severe hypothalamic dysfunction, assisted reproductive technologies like IVF with donor eggs offer paths to parenthood.
The key is early action. The sooner anovulation is identified and treated, the better the fertility outcomes.
Frequently Asked Questions (FAQs)
Can you have a period without ovulating?
Yes. Anovulatory bleeding can mimic a period, but it is caused by estrogen fluctuations rather than the progesterone drop that follows true ovulation.
How do I know if I am ovulating?
Track your basal body temperature for a sustained rise after mid-cycle, observe egg-white cervical mucus, and use ovulation predictor kits. A mid-luteal blood progesterone test is the most reliable confirmation.
Is it common to not ovulate every cycle?
Yes. Around 30% of women have experienced at least one anovulatory cycle. Occasional anovulation is normal, but chronic anovulation needs medical evaluation.
Can stress stop ovulation?
Yes. Chronic stress elevates cortisol, which suppresses GnRH and disrupts the hormonal cascade needed for ovulation. Stress management can help restore ovulation in some women.
Does PCOS always cause anovulation?
Not always, but PCOS is the most common cause of chronic anovulation. Not every woman with PCOS will be anovulatory in every cycle, but irregular or absent ovulation is a hallmark of the condition.
Can losing weight restore ovulation?
Yes. For women who are overweight, losing as little as 5% of body weight can significantly improve hormone balance and restore ovulation. Weight management is often a first-line treatment.
What is the best test to confirm ovulation?
A mid-luteal progesterone blood test (done around day 21) is the most reliable. Levels above 3 ng/mL confirm that ovulation occurred. Transvaginal ultrasound is the most definitive method.
Can you get pregnant during an anovulatory cycle?
No. Pregnancy requires a released egg to be fertilized. Without ovulation, conception is not possible in that cycle. Treatment is necessary to restore ovulation for natural conception.
How long does it take to restore ovulation naturally?
It varies by cause. Stress and weight-related anovulation can resolve within 1 to 3 months with lifestyle changes. Hormonal conditions like PCOS or thyroid disorders may require medical treatment and several months to fully normalize.
When should I see a fertility specialist about not ovulating?
See a specialist if you are under 35 and have been trying to conceive for 12 months without success, or if you are over 35 and have been trying for 6 months. Also seek evaluation for consistently irregular cycles, suspected PCOS, or any absence of ovulation signs.
Conclusion
Why am I not ovulating but having periods is a question that deserves a clear, science-backed answer — and in 2026, women have more tools and treatments available than ever before.
Anovulation is common, affecting around 30% of women at some point, and it is one of the leading causes of female infertility. The good news is that with proper diagnosis, most cases are highly treatable.
From lifestyle adjustments like weight management, stress reduction, and targeted nutrition, to medical options like letrozole, Clomid, and ovulation induction, there are real solutions for every cause.
If you suspect you are not ovulating, do not wait. Track your symptoms, speak with your doctor, and get the hormonal testing you need. Early action leads to better outcomes — for your fertility and for your overall reproductive health.

