Why do hemorrhoids bleed is one of the most searched health questions — and for good reason. Seeing blood after a bowel movement can be frightening.
Hemorrhoids, also known as piles, are swollen veins in the rectum or around the anus that affect an estimated 1 in 20 Americans.
When these veins become irritated, damaged, or ruptured, they bleed. Understanding why this happens — and what you can do about it — is the first step toward real relief.
What Are Hemorrhoids?
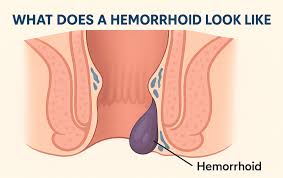
Hemorrhoids are cushions of blood vessels, connective tissue, and muscle located at the end of the rectum and around the anus. Everyone has them. They only become a problem when they swell, enlarge, or get irritated.
There are two main types: internal hemorrhoids, which form inside the rectum and are usually painless but prone to bleeding, and external hemorrhoids, which develop under the skin around the anus and can cause pain, itching, and sometimes bleeding.
A third type — thrombosed hemorrhoids — occurs when a blood clot forms inside an external hemorrhoid. This causes intense pain, significant swelling, and a hard purple or blue lump near the anus.
Why Do Hemorrhoids Bleed?
Hemorrhoids bleed when the swollen veins inside or around the anus become irritated, stretched, or ruptured. The thin walls of these blood vessels are fragile. When too much pressure is applied — through straining, hard stool, or prolonged sitting — the vessel wall can tear or burst, releasing bright red blood.
The bleeding is usually painless for internal hemorrhoids because there are no pain-sensing nerves in that part of the rectum. External hemorrhoids, when they bleed, tend to also cause pain or discomfort.
Bright red blood on toilet paper, in the toilet bowl, or on the surface of stool is the most common sign. If the blood is dark red or maroon, it may indicate bleeding higher up in the digestive tract, and a doctor should be seen immediately.
Top Causes of Hemorrhoid Bleeding
Understanding what triggers bleeding helps prevent it. Here are the most common causes:
Straining During Bowel Movements
Straining is the number one cause of hemorrhoid bleeding. When you push hard during a bowel movement, pressure builds up in the rectal veins. This causes the hemorrhoid walls to stretch and eventually rupture, resulting in bleeding.
Chronic constipation is the main driver of straining. Hard, dry stools force you to push longer and harder, multiplying the pressure on hemorrhoidal tissue.
Chronic Constipation
Constipation causes hard, compacted stools that scrape against the delicate walls of swollen hemorrhoids as they pass. This physical trauma is enough to break blood vessels and trigger bleeding.
A low-fiber diet, dehydration, and sedentary habits are the most common reasons behind chronic constipation. Increasing daily fiber intake to 25–35 grams can dramatically reduce this risk.
Diarrhea
Loose, frequent stools irritate the anal canal repeatedly throughout the day. Each bowel movement rubs against inflamed hemorrhoidal tissue, causing micro-tears that bleed.
Chronic diarrhea from conditions like irritable bowel syndrome (IBS) or infections can cause persistent hemorrhoid flare-ups with ongoing bleeding.
Prolonged Sitting
Sitting for long periods — especially on the toilet — increases pressure on the rectal veins. The weight of the body concentrates directly on the anal region, restricting blood flow and causing veins to swell.
Sitting on the toilet for more than a few minutes while scrolling your phone is one of the worst habits for hemorrhoid health.
Pregnancy
Pregnancy is a major risk factor for hemorrhoid bleeding. The growing uterus places direct pressure on the rectal veins, while hormonal changes relax blood vessel walls, making them more prone to swelling.
Constipation, which is common during pregnancy, compounds the problem. Hemorrhoid bleeding during pregnancy typically improves after delivery but should still be evaluated by a doctor.
Heavy Lifting
Lifting heavy objects causes a sudden spike in abdominal pressure, similar to straining during a bowel movement. This surge pushes blood into the hemorrhoidal veins and can cause them to rupture.
Improper lifting technique without core bracing significantly increases this risk.
Aging and Weakened Tissue
As the body ages, the connective tissue that supports hemorrhoidal cushions weakens. This allows the veins to sag, stretch, and prolapse more easily. More than half of people over age 50 experience symptomatic hemorrhoids.
Weaker vessel walls also mean that even minor irritation can cause bleeding in older adults.
Low-Fiber Diet
A diet lacking in fruits, vegetables, whole grains, and legumes produces hard stools that are difficult to pass. This directly contributes to straining, constipation, and the physical trauma that causes hemorrhoids to bleed.
Processed foods, excess red meat, and low fluid intake all worsen the problem.
Hemorrhoid Types and Bleeding Risk
| Hemorrhoid Type | Location | Bleeding Risk | Pain Level |
|---|---|---|---|
| Internal (Grade I–II) | Inside rectum | High — painless bleeding | None to mild |
| Internal (Grade III–IV) | Prolapsed outside | High — with prolapse | Moderate |
| External | Under anal skin | Moderate | Moderate to severe |
| Thrombosed External | Around anus | Moderate — if ruptured | Severe |
Internal hemorrhoids are the most common source of painless, bright-red rectal bleeding. External hemorrhoids bleed less frequently but are more painful when they do.
What Does Hemorrhoid Bleeding Look Like?
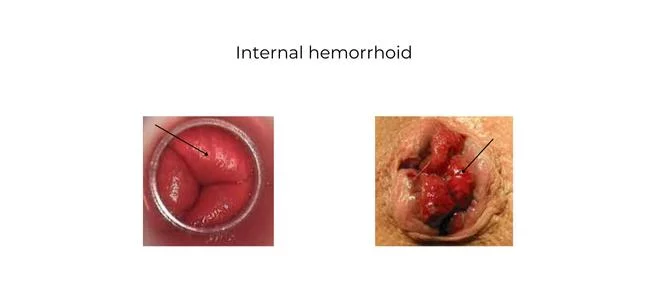
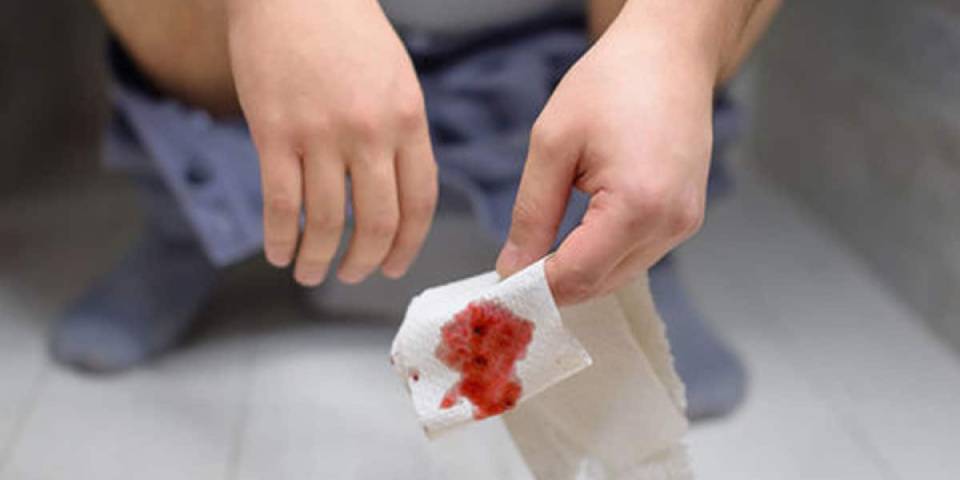
Normal hemorrhoid bleeding is a small amount — typically a few drops — of bright red blood seen on toilet paper or in the toilet bowl after a bowel movement.
The blood should not be mixed throughout the stool. If blood is dark, tarry, or present in large amounts, it is not typical of hemorrhoids and requires urgent medical evaluation to rule out conditions like colorectal cancer, IBD, or diverticular disease.
When Does Hemorrhoid Bleeding Become Dangerous?
Hemorrhoid bleeding is rarely life-threatening but should not be ignored in certain situations. Here is when you need to seek medical attention:
See a doctor if you notice:
- Bleeding lasting more than 7 days without improvement
- Heavy bleeding that does not stop within a few minutes
- Blood mixed throughout the stool (not just on the surface or paper)
- Dark red, maroon, or black stool
- Dizziness, lightheadedness, or fatigue with bleeding
- Severe anal pain alongside bleeding
- Fever or signs of infection
Chronic hemorrhoid bleeding can also lead to iron-deficiency anemia over time, causing fatigue, weakness, and shortness of breath — even if each individual bleed seems small.
Quick Relief for Bleeding Hemorrhoids at Home
Most cases of hemorrhoid bleeding can be managed safely at home. The goal is to reduce pressure on the swollen veins, soften stools, and soothe irritated tissue.
Sitz Bath
A sitz bath is one of the most effective home treatments for bleeding hemorrhoids. Fill a shallow basin or bathtub with a few inches of warm (not hot) water. Soak the anal area for 15–20 minutes, two to three times daily — especially after bowel movements.
Adding Epsom salt or baking soda can enhance the anti-inflammatory effect. Sitz baths reduce swelling, ease pain, and promote healing of irritated tissue without any medication.
Increase Fiber Intake
Boosting dietary fiber is the single most important long-term step for preventing hemorrhoid bleeding. Fiber softens stool, making it easier to pass without straining.
High-fiber foods to add to your diet:
| Food Category | Examples | Fiber Per Serving |
|---|---|---|
| Fruits | Apples, pears, berries | 3–5g |
| Vegetables | Broccoli, carrots, leafy greens | 2–4g |
| Legumes | Beans, lentils, chickpeas | 6–8g |
| Whole Grains | Oats, brown rice, whole wheat | 3–6g |
| Fiber Supplements | Psyllium husk, methylcellulose | 3–5g per dose |
Target 25–35 grams of fiber daily. Increase intake gradually to avoid bloating and gas.
Stay Well Hydrated
Water is essential for preventing the hard stools that cause hemorrhoid bleeding. Aim for 8–10 glasses of water per day.
Proper hydration works together with fiber to keep stools soft and easy to pass. Dehydration — even mild — can quickly undo the benefits of a high-fiber diet.
Cold Compress
Applying an ice pack or cold compress wrapped in a clean cloth to the anal area for 10–15 minutes at a time can reduce swelling and numb the pain associated with bleeding hemorrhoids.
Repeat several times throughout the day. Never apply ice directly to the skin. Cold reduces inflammation quickly and provides fast temporary relief.
OTC Hemorrhoid Creams and Ointments
Over-the-counter topical products can reduce irritation, itching, and minor bleeding. Look for creams containing:
- Hydrocortisone — reduces inflammation
- Witch hazel — natural astringent that constricts blood vessels
- Pramoxine — numbs pain and discomfort
- Zinc oxide — protects and soothes irritated skin
- Aloe vera — calms inflammation and promotes healing
Products like Preparation H, Tucks pads, and witch hazel pads are widely available and effective for short-term symptom relief.
Gentle Cleaning Habits
Aggressive wiping with dry, rough toilet paper is a direct cause of hemorrhoid irritation and bleeding. Switch to soft, unscented toilet paper or unscented moist wipes after bowel movements.
Patting — not rubbing — the anal area is essential. Alternatively, rinsing with warm water using a bidet or handheld sprayer is the gentlest and most effective cleaning method.
Avoid Straining and Long Sitting
Go to the bathroom as soon as you feel the urge — do not delay. Postponing a bowel movement makes stool harder and drier, increasing straining when you do go.
Limit toilet time to under 5 minutes. Leave your phone outside the bathroom. Elevating your feet on a small stool while sitting on the toilet (mimicking a squat position) can reduce straining significantly.
Stool Softeners and Laxatives
If constipation is driving your hemorrhoid bleeding, a short course of over-the-counter stool softeners like docusate sodium can help. These make stools softer without causing the cramping that stimulant laxatives produce.
Osmotic laxatives like MiraLax can also help by drawing water into the colon. These are safe for short-term use while you adjust your diet.
Medical Treatments for Persistent Bleeding Hemorrhoids
When home treatment is not enough — or if bleeding continues beyond 7 days — medical procedures can provide more definitive relief:
Rubber Band Ligation
Rubber band ligation is the most commonly used office procedure for internal hemorrhoids. A doctor places a small rubber band around the base of the hemorrhoid, cutting off its blood supply. The hemorrhoid shrivels and falls off within 3–10 days.
This procedure has an 89% success rate and is suitable for Grade II and Grade III internal hemorrhoids. It is typically done without anesthesia in the office.
Sclerotherapy
Sclerotherapy involves injecting a chemical solution into the hemorrhoid tissue, causing it to shrink and scar over. This cuts off blood supply and shrinks the hemorrhoid over several weeks.
It is effective for smaller internal hemorrhoids and may require multiple treatment sessions over several weeks.
Infrared Coagulation (IRC)
IRC uses focused infrared light or heat to create scar tissue that cuts off the blood supply to the hemorrhoid. It is effective for Grade I and II internal hemorrhoids and is performed in the office setting.
IRC is valued for its safety profile and minimal recovery time in outpatient settings.
Hemorrhoidectomy
Surgical hemorrhoid removal (hemorrhoidectomy) is reserved for large, severely prolapsed, or recurring hemorrhoids that do not respond to other treatments. It carries a 2–10% recurrence rate — the lowest of any option — but involves a recovery period of 9–14 days.
This is the gold standard for Grade III and IV hemorrhoids or mixed (internal and external) hemorrhoids requiring definitive treatment.
Hemorrhoid Stapling (PPH)
Procedure for prolapse and hemorrhoids (PPH) uses a circular stapling device to remove a ring of excess tissue and reposition prolapsed hemorrhoids. It is less painful than traditional hemorrhoidectomy but has a slightly higher recurrence rate.
It is most commonly used for prolapsed internal hemorrhoids.
Prevention: How to Stop Hemorrhoids From Bleeding Again

Preventing recurrence is as important as treating the current episode. These evidence-based habits reduce hemorrhoid flare-ups long-term:
Diet and Hydration: Eat a fiber-rich diet daily (25–35g) and drink 8–10 glasses of water. Reduce processed foods, red meat, alcohol, and caffeine, which worsen constipation.
Exercise Regularly: Walking 30 minutes daily stimulates bowel activity and reduces pressure on pelvic veins. Avoid heavy weightlifting or high-impact exercises during active hemorrhoid flare-ups.
Healthy Toilet Habits: Go when you feel the urge. Never strain. Spend less than 5 minutes on the toilet. Use a footstool to optimize your posture. Clean gently with soft, moist wipes or water.
Maintain a Healthy Weight: Excess body weight increases abdominal pressure and puts additional strain on rectal veins. Weight loss significantly reduces hemorrhoid recurrence in overweight individuals.
Manage Bowel Habits: Treat diarrhea and constipation promptly. Both extremes damage hemorrhoidal tissue. Consistent, soft, easy-to-pass stools are the goal.
Hemorrhoid Bleeding vs. Other Rectal Bleeding
Not all rectal bleeding is from hemorrhoids. It is important to distinguish hemorrhoid bleeding from more serious causes:
| Condition | Blood Color | Pattern | Pain |
|---|---|---|---|
| Hemorrhoids | Bright red | On paper or in bowl | None to mild |
| Anal Fissure | Bright red | On paper, with stool | Sharp pain |
| Colorectal Polyp | Bright to dark red | Mixed in stool | Usually none |
| Colorectal Cancer | Dark red / maroon | Mixed in stool | May be none |
| Diverticular Disease | Bright or dark red | Large amounts | Usually none |
| IBD (Crohn’s/UC) | Dark red | Mixed in stool | Cramping |
Any rectal bleeding that does not fit the typical hemorrhoid pattern — small amount, bright red, on the surface — warrants a doctor’s evaluation and possibly a colonoscopy to rule out other causes.
Frequently Asked Questions (FAQs)
Why do hemorrhoids bleed without pain?
Internal hemorrhoids bleed without pain because they form above the dentate line in the rectum, where there are no pain-sensing nerve endings. The only symptom is often bright red blood on toilet paper or in the bowl.
Is hemorrhoid bleeding serious?
Small amounts of bright red blood from hemorrhoids are usually not serious. However, persistent, heavy, or recurring bleeding should be evaluated by a doctor to rule out other conditions and prevent anemia.
How long does hemorrhoid bleeding last?
Hemorrhoid bleeding typically stops within a few days with basic home care. If bleeding continues beyond 7 days or keeps returning, it is time to consult a healthcare provider for proper treatment.
Can hemorrhoids bleed without a bowel movement?
Yes. Hemorrhoids can bleed from activities like prolonged sitting, heavy lifting, excessive wiping, or even physical activity that increases abdominal pressure, all without a bowel movement occurring.
What stops hemorrhoid bleeding fast at home?
A cold compress, warm sitz bath, witch hazel pads, and OTC hemorrhoid cream are the fastest home remedies. Increasing water and fiber intake helps prevent further bleeding by softening stools.
Does drinking water help hemorrhoid bleeding?
Yes. Staying well hydrated softens stools, reduces straining, and eases bowel movements — directly reducing the friction and pressure that causes hemorrhoids to bleed.
Can thrombosed hemorrhoids bleed a lot?
Yes. A thrombosed hemorrhoid contains a blood clot. If it ruptures, it can bleed significantly — sometimes for several minutes. This type of bleeding should be evaluated by a doctor promptly.
Is bright red blood always from hemorrhoids?
Not always. Bright red blood on toilet paper often indicates hemorrhoids or an anal fissure, but it can also come from polyps or other rectal conditions. Persistent bright red rectal bleeding always warrants medical evaluation.
When should I go to the ER for hemorrhoid bleeding?
Go to the ER if you experience heavy rectal bleeding that does not stop, blood clots in the toilet, dizziness, weakness, rapid heartbeat, or if you feel faint. These may indicate significant blood loss.
Can I exercise with bleeding hemorrhoids?
Light walking is safe and actually beneficial. Avoid heavy lifting, intense cardio, or exercises that increase abdominal pressure until bleeding resolves. Exercise helps improve bowel regularity, which reduces future bleeding.
Conclusion
Why do hemorrhoids bleed comes down to one core answer: swollen, fragile veins under pressure. Whether the cause is constipation, straining, pregnancy, or prolonged sitting, the result is the same — thin hemorrhoidal vessel walls break and release blood.
The good news is that most hemorrhoid bleeding responds well to simple, consistent home care. A high-fiber diet, adequate hydration, sitz baths, gentle cleaning habits, and OTC creams can resolve the majority of cases within a week.
For persistent or recurring bleeding, office-based procedures like rubber band ligation offer fast, effective, minimally invasive relief.
The key is not to ignore the symptom. With the right approach, hemorrhoid bleeding is both treatable and preventable — giving you lasting comfort and peace of mind.

